How do clinical trials work? Are they free? Am I eligible? Being Patient answers readers' most frequently asked questions about clinical trials for Alzheimer's and dementia treatments, diagnostics and more.
Clinical trials and studies scientific experiments that investigate new treatments, lifestyle interventions, or risk factors for developing a disease like Alzheimer’s or dementia. By becoming a participant, you help forward new insights and treatments for the disease.
These trials and studies come in different shapes and sizes. Understanding the type of research you’re participating in will help you understand its purpose and whether it is right for you.
Clinical trials and studies are run from research centers or universities. Each study is headed by a principal investigator who is usually a physician and researcher, along with many doctors, nurses, and other healthcare staff.
They may also be sponsored by pharmaceutical companies testing out new drugs. Descriptors for the trial provide information about how far along a drug is in its development, or whether the trial involves a placebo — a sham version of the treatment to help scientists test its effects — is involved. (We’ll take a closer look at that below.)
In general, there are two main clinical studies and trials, with many different design variations and goals. The goals, protocols, and other information about a clinical trial or study is posted before the start of the trial on clinicaltrials.gov.
Here’s a quick run-down.
What is a clinical trial?
In a clinical trial, the general public signs up to help scientists learn critical information about illnesses and the interventions that treat them. These interventions might be medical, surgical, or behavioral. In the Alzheimer’s research space, there is much discussion of a number of ongoing clinical trials testing whether experimental, new drugs can help slow down or stop Alzheimer’s disease progression. There are also clinical studies that look at Alzheimer’s effects on the brain, and the factors that may cause it, make it more likely, or help prevent it.
The goal of such studies is to gather vast amounts of data that then helps researchers understand whether, for example, a particular dementia treatment is safe and effective for people living with dementia — and whether it is better than other available treatments.
Some of the interventions that are tested in trials include:
- Drugs. Currently, there are several clinical drug trials testing whether anti-amyloid drugs like lecanemab are “disease modifying.” In other words, these trials are testing whether a drug can actually change the course of the disease, as opposed to only treating its symptoms.
- Medical devices. Medical device trials test devices. The devices category includes new diagnostics like Alzheimer’s blood tests which are currently being developed to provide earlier Alzheimer’s diagnosis for patients and, ultimately, better treatment and care.
- Procedures. In the dementia research space, trials that test medical procedures might explore new ways of measuring cognitive function in people with Alzheimer’s and other forms of dementia. Tests that provide more accurate information about cognitive function could lead to improvements in diagnosis and treatment.
- Behavioral interventions. There are also clinical trials that test certain “behavioral interventions,” like lifestyle changes, and their effects on health or illnesses. For example, a clinical behavioral intervention trial from Finland used a combination of interventions including dietary changes and exercise to examine whether these behaviors reduced participants’ risk of developing dementia. These clinical trials can last for several years.
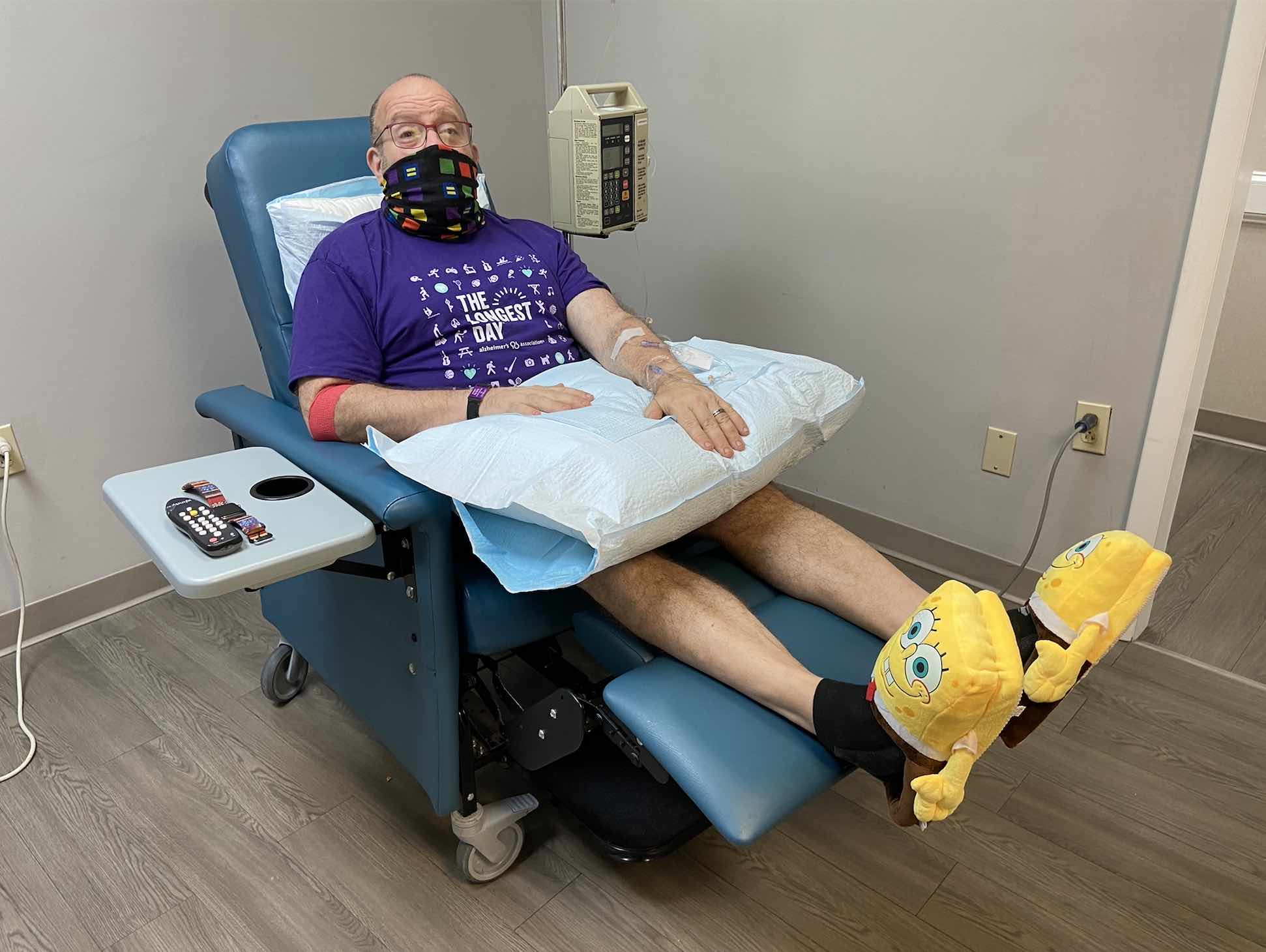
Medical interventions go through different phases of clinical trials. Each phase gathers information about safety and efficacy, which is then reviewed by regulating agencies. In the U.S., the agency is the Food and Drug Administration (FDA), which decides whether to approve new drugs and diagnostic tools so that they can become available to the general public. These are the different phases:
- Phase 1. This phase is the earliest trial for any medical intervention. It is conducted in a small group of healthy participants to assess safety and, in the case of drug testing, appropriate dosage.
- Phase 2. This is the middle phase of investigation and often the first phase where participants have a specific disease or condition. A Phase 2 trial provides information about preliminary effectiveness and dosages in a larger group of participants.
- Phase 3. Phase 3 trials, sometimes combined with Phase 2 trials, test whether a drug works in a larger cohort of participants with a disease. Often, this pits a new intervention against the gold standard treatment for the condition or a placebo.*
What are observational studies?
Observational studies are exactly what they sound like: They are very “hands-off.” The researchers do not introduce any new interventions or treatments to the participants. Instead, the researchers stand back, observe people over a long period of time, and gather data to answer questions like “Does drinking diet soda increase the risk of developing dementia?” or “Does viagra cut dementia risk?”
This can help explain the effects of certain interventions in the real world, sometimes providing evidence that drugs used for one indication may also reduce the risk or slow the progression of cognitive decline. If any promising drugs are found through this method, they are tested again in a more rigorous clinical trial.
Who is eligible for a clinical trial?
Each study or trial has a plan that outlines exactly what kind of participants a study is recruiting for.
A list of necessary requirements for participating in such a trial is called the eligibility criteria.
In the case of an Alzheimer’s or dementia trial, eligibility criteria may include:
- Genetic risk factors like APOE4
- The stage of your disease and severity of the symptoms
- Presence of Alzheimer’s-associated biomarkers in your blood or brain
- Age
- Gender
There are also exclusion criteria for many clinical trials. For example, if you are taking other medications, such as blood thinners, or you have a co-occurring illness or condition, you may be excluded from participating in a clinical trial.
Are clinical trials free?
Typically, participants are reimbursed for any costs that might be incurred by participating in a clinical trial, such as the cost of procedures during the screening process, or travel to trial sites. Some clinical trials also pay compensation to the participants throughout the trial.
However, this is not always the case. From a patient’s perspective, these trials often don’t cost them anything. Trial sponsors are typically reimbursed for procedures that are offered during the trial by Medicare if these procedures are eligible. The sponsor might still pay for the procedures so participants don’t incur additional costs.
The first stage of any trial involves a screening process which can sometimes last weeks or months, which helps trial administrators determine whether a potential participant may be eligible. Sometimes, a diagnosis is required to enter the screening process, according to Terrence Casey, director of communications and outreach at the Penn Memory Center. “It depends on the trial and the inclusion and exclusion criteria as determined by the study sponsor,” Casey told Being Patient.
Drug trials are often seeking people in a certain stage of a certain disease — for example, early-stage Alzheimer’s disease. However, Alzheimer’s and other forms of dementia are notoriously difficult to accurately diagnose. So, part of that eligibility determination depends on the confirmation of a patient’s diagnosis. This trial eligibility screening process usually doesn’t cost the patient anything.
The bottom line: The situation may differ, from trial to trial, and sometimes, depending on diagnosis status, from patient to patient. While many trials do reimburse participants for the trial expenses, this is not always the case. Ask your trial administrator at the start of the eligibility screening process whether there will be out-of-pocket expenses for you in order to participate.
What’s a placebo?
To better understand whether drugs are effective without any bias, often, participants would be randomized to different treatment groups at the start of the trial. One group will receive a treatment while another group would receive a dummy that looks just like the treatment, which is called a “placebo” or “sham” treatment.
A placebo is a sugar-pill or other substitute given in lieu of a drug. In an Alzheimer’s drug trial, for example, all the participants in the study of a monoclonal antibody receive an infusion. But only one group of participants will receive an infusion with the drug being tested. A sham treatment is a simulation of a procedure, such as magnetic stimulation, that makes it hard for a participant to tell whether they receive the actual treatment.
As a best practice, many Phase 2 and Phase 3 clinical trials will withhold this information from participants and clinicians until the very end.
If you sign up for a single-blinded trial, you will not learn until the end whether you receive the treatment being tested, or the placebo. In a double-blinded trial, neither the clinicians nor the participants will know whether they receive the treatment or the placebo.
These practices make the results of a clinical trial more robust by controlling for the placebo effect: Clinician and patient expectations that can influence the results of the study.
Are clinical trials ethical?
The United States has a dark history when it comes to medical experimentation. Events like the Syphilis Study at Tuskegee or the mistreatment of Henrietta Lacks and the cloning of her cancer cells were unethical and exploitative of people of color.
Today, there are safeguards in place that protect participants in clinical trials more than ever before. Months or years before anyone is ever recruited, researchers who want to conduct a study must fill out forms and explanations of the study which are then reviewed by an institutional review board.
These boards consist of doctors, researchers, and people outside the medical community. Their goal is to make sure the trial is well designed so that it does not cause any unnecessary harm to participants.
The second line of protection is called informed consent. This helps participants and their families weigh the risks and benefits of participating in the study. Throughout this process, the researchers also assess how well a participant understands the study.
Once everything is clear, the participant can choose to sign a consent form and join the trial. Participants can withdraw their consent at any time, even if the trial has not yet ended.
Should I join a clinical trial?
There are some risks to participating in any clinical trial or study. If the trial is randomized and blinded, you might not even receive the treatment. You could also experience some side effects. There is the risk that the treatment may not work.
However, everyone who participates furthers our understanding of Alzheimer’s disease and dementia. Even studies where a drug or intervention is ineffective provide valuable information for researchers. You could also receive a treatment for a disease before it is available anywhere else. You will receive more frequent check ups. Importantly, you can also feel empowered by taking an active role in your health.
Ultimately, deciding whether to participate in a study is a decision for you and your family. However by participating you can help advance the science of Alzheimer’s disease and dementia, helping researchers close in on a cure.




My husband would like to participate in any clinical trials for Alzheimer’s. He was diagnosed by a neurologist in Boise, ID with dementia and she said 92% of the time that is Alzheimer’s. This was just over a year ago and his memory has been declining slowly. His main problem is with numbers, dates, times, anything to do with numbers. He just turned 77 and otherwise is in great health.