A Lapse in the Brain’s Security System Might Cause Alzheimer’s—And There’s a Drug to Help
According to new research, it might be a breakdown of the blood-brain barrier and leaky blood vessels that point to Alzheimer's before anything else.
A ‘leaky’ brain may be the first sign of Alzheimer’s in the brain—not the presence of beta-amyloid proteins or tau tangles, as researchers previously thought, a new study by the University of Southern California has found.
Researchers have long thought that beta-amyloid, a protein that accumulates in the brains of Alzheimer’s, was the first sign of Alzheimer’s, appearing in clumps long before symptoms like memory loss begin. But according to research published in the journal Nature, it might be a breakdown of the blood-brain barrier and leaky capillaries in the brain that point to Alzheimer’s before anything else.
The blood-brain barrier is like the brain’s security system—it acts as a stable barrier between the brain and blood flow, only letting certain things pass through. In the past, that’s been a challenge for scientists who aimed to deliver drugs that could potentially stop or slow down diseases like Alzheimer’s.
For this study, 161 patients with an average age of 45 were recruited. All had either no signs of cognitive impairment or very early signs of mild cognitive impairment. At the beginning of the study, researchers conducted cognitive tests on the patients and measured their brain capillaries using neuroimaging and samples of cerebrospinal fluid.
The five-year study found that those with more capillary damage, or leakage, also had the worst memory problems. However, there was no relation between cognitive problems and beta-amyloid or tau proteins—the two biomarkers scientists use to officially diagnose Alzheimer’s and gauge a person’s likelihood of developing the disease.
“The fact that we’re seeing the blood vessels leaking, independent of tau and independent of amyloid, when people have cognitive impairment on a mild level, suggests it could be a totally separate process or a very early process,” said senior author Berislav Zlokovic, director of the Zilkha Neurogenetic Institute at the Keck School of Medicine of USC. “That was surprising that this blood-brain barrier breakdown is occurring independently.”
A healthy blood-brain barrier is made up of tightly woven blood vessels that keep metals, other cells and toxic substances from entering and damaging the brain. But as we age, those cells can loosen, making the blood vessels penetrable.
Leaky blood vessels may provide an avenue through the blood-brain barrier.
Image: Arthur Toga Lab/Keck School of Medicine of USC
“If the blood-brain barrier is not working properly, then there is the potential for damage,” said co-author Arthur Toga, director of the USC Stevens Neuroimaging and Informatics Institute at the Keck School of Medicine. “It suggests the vessels aren’t properly providing the nutrients and blood flow that the neurons need. And you have the possibility of toxic proteins getting in.”
But the patients in the study with leaky blood vessels may be in luck: Another study released by USC showed that an experimental stroke drug called 3K3A-APC may help repair those vessels. The drug reduces inflammation and protects the cells lining blood vessel walls from death and degeneration in stroke patients. In an experiment with mice engineered to have Alzheimer’s, the drug was able to reduce the build-up of beta-amyloid and prevent memory loss.
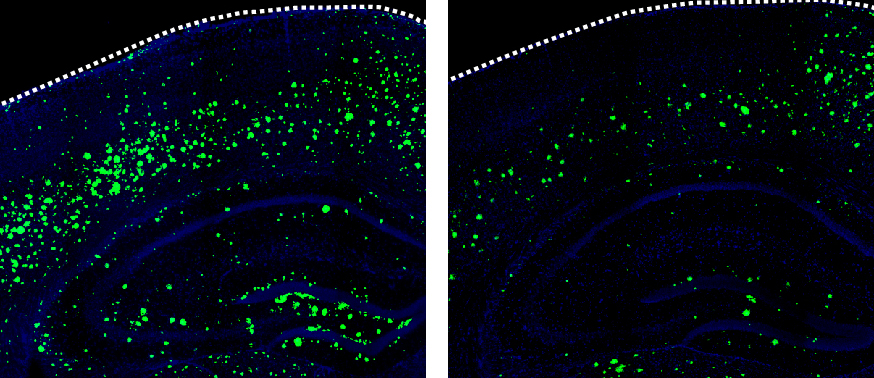
The stroke drug 3K3A-APC (right) greatly reduces the amount of beta-amyloid (green) that accumulates in the brains of mice that develop Alzheimer’s-like symptoms compared with no treatment (left).
Image: Lazic et al., 2019
“Because of its neuroprotective, vasculoprotective, and anti-inflammatory activities in multiple models of neurological disorders, we investigated whether 3K3A-APC can also protect the brain from the toxic effects of [beta-amyloid] toxin in a mouse model of Alzheimer’s disease,” says Berislav V. Zlokovic, director of the Zilkha Neurogenetic Institute at the Keck School of Medicine, University of Southern California.
However, both study results come with cautions. For the first study, researchers emphasized that their findings represented a small snapshot in time. They don’t yet know how a leaking blood-brain barrier might affect the development of Alzheimer’s later down the line. And because the stroke drug study was performed on mice, it’s difficult to say if humans would have the same outcome. But both studies disrupt what was considered near-fact about the beginning signs of Alzheimer’s in the brain.
“The results were really kind of eye-opening,” said first author Daniel Nation, an assistant professor of psychology at the USC Dornsife College of Letters, Arts and Sciences. “It didn’t matter whether people had amyloid or tau pathology; they still had cognitive impairment.”











can this leaky brain be reversed in a person with Vascular Dementia?
Your article says ‘and there’s a drug to help’. However, no information on this drug?? Please enlarge. This is not helpful as there must be very many people hoping for a ‘helpful drug to be found. J
Hello Jane, the ninth paragraph has the information you are looking for. ~ Thank you.