A Pacemaker for Parkinson’s, Alzheimer’s? Deep Brain Stimulation, Explained
Deep brain stimulation involves implanting a pacemaker-like device in the brain. It's already in use for diseases like Parkinson's. Now, scientists are exploring these high-tech brain-zapping techniques to treat Alzheimer’s?
In 2013, 29-year-old Ben Stecher went to the doctor with concerning symptoms — he felt like he was moving in slow-motion, and his hands would occasionally shake uncontrollably.
His doctors diagnosed him with Parkinson’s, a neurodegenerative disease that causes cells in a small part of the brain called the substantia nigra to die off. In Stecher’s brain, these cells were no longer producing important chemical signals for helping the body move, causing a slew of other problems to develop with balance, involuntary tremors, and posture. He was put on medication that would help his brain replace these chemical signals, but they wouldn’t get at the root cause of Parkinson’s, and they wouldn’t stop its progression.
Eight years later, Stecher was on some 20 different medications to help control his Parkinson’s, and still, his symptoms were growing worse. Many people like Stecher also experience what are called “ON” and “OFF” fluctuations where the medication works sometimes and other times it doesn’t.
He began to experience uncontrollable writhing that could last for an hour. One of his medications might tamp them down for a brief moment, and then wear off.
In June 2021, Stecher struck out on a bold, different course of treatment: He worked with his surgeon to have two six-inch-long metal spikes implanted, deep into his brain. These were neuromodulation devices — and they would would serve, essentially, as a pacemaker, zapping parts of Stecher’s brain back to work.
This surgical treatment, also called deep brain stimulation (DBS), helped reel in some of Stecher’s worsening symptoms, particularly the slowness of movement and muscle cramping. DBS is a form of neuromodulation, a treatment that involves stimulating the brain’s nerve cells.
Now, Stecher told Being Patient, most of his symptoms have improved, while the amount of medication he needs to take daily has been dramatically reduced. In fact, the devices, so far, have been life-changing.
“When properly optimized, it’s brought my baseline ‘OFF’ up to about 90 percent of a normal person’s,” Stecher said. “Most people I interact with during those times do not even know anything is wrong with me.”
Stecher is far from the first person to receive the surgery. Since it was first approved for treating Parkinson’s tremors 1997, there are more than 160,000 people worldwide that use DBS to help them manage their symptoms with 12,000 people getting the surgery each year. This technology has also expanded to help people with severe forms of depression, obsessive compulsive disorder, epilepsy, and is being studied as a way to augment memory and brain function in Alzheimer’s disease. So how does it work?
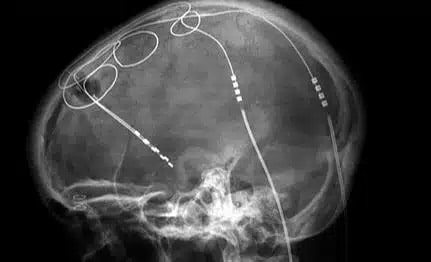
Image: Dr. Craig Hacking, A. Prof Frank Gaillard [CC BY-SA 4.0 via Wikimedia Commons]
Deep brain stimulation for Parkinson’s disease
Parkinson’s is a neurodegenerative disease that can progress to Lewy body dementia. It causes cells in a small part of the brain called the substantia nigra, that produce a chemical messenger called dopamine, to die off.
Many people associate dopamine with motivation or the little boost of happiness people get when they see notifications on their social media apps. But dopamine is also involved in regulating movement. As the disease progresses, the brain isn’t producing enough dopamine so people develop problems with balance, involuntary tremors, slowness of movement, and difficulty walking.
“When properly optimized, it’s brought my baseline ‘OFF’ up to about 90 percent of a normal person’s. Most people I interact with during those times do not even know anything is wrong with me.”
Researchers developed a surgical treatment called DBS which involves inserting a piece of metal into the brain, connected to a battery implanted under the chest, that will act as a pacemaker to stimulate a specific group of cells, treating symptoms of the disease. The part of the brain that is stimulated depends on a patient’s symptoms and needs. For example, people who experience a lot of side effects from medication might have the DBS inserted into the subthalamic nucleus which can reduce how much of their medications they need to take.
DBS was approved by the FDA in 1997 to treat Parkinson’s tremors, in 2002 to treat advanced symptoms of the disease, and once again in 2016 for treating the earlier stages of Parkinson’s in people whose symptoms don’t respond to medications.
Side effects of DBS for Parkinson’s
Some people who receive DBS for Parkinson’s will experience side effects tingling in their face, arms or legs, a feeling of pulling in their muscles, loss of balance, speech or vision problems, and headaches. However, some of these side effects go away as the level of stimulation provided by the device can be adjusted.
How much does DBS cost for Parkinson’s disease?
This treatment might cost about $40,000 for the initial surgery. Patients may need a second surgery to replace the power source if the battery runs out. Including all the care and follow-ups, researchers estimated a cost of up to $180,000 over five years.
DBS for Alzheimer’s disease
Alzheimer’s disease damages and kills brain cells, which disrupts their ability to send chemical and electrical messages back and forth. When enough of these messages misfire, it causes noticeable symptoms like personality changes, forgetfulness, and difficulty thinking. There are treatments, like cholinesterase inhibitors, designed to address these symptoms by altering the levels of chemical messengers — called acetylcholine — in the brain.
These drugs compensate for the chemical disruptions in the Alzheimer’s brain, but what about fixing some of the electrical problems? Enter DBS.
Scientists are now testing this technology in clinical trials, and researchers are using what they learn to develop less invasive methods for stimulating the brain.
“With DBS, we’re just trying to tap into the potentially an abnormal circuit and augment it — not [to] reverse the disease,” Dr. Darrin Lee, a neurosurgeon and assistant professor at the the University of South California’s Keck School of Medicine, told Being Patient, “but more of [to reverse] the symptoms.”
According to Lee, most research so far is looking at two very specific small brain regions.
The first region lies within a part of the brain called the fornix. Here, scientists are using these little metal implants to light up a bundle of cells — known as a “white matter tract” — that carry electrical information like wires from one place to the next.
“That seems to be important in memory,” Lee said of this part of the fornix.
The second tiny focus area for these experimental Alzheimer’s therapies is the nucleus basalis of Meynert, a group of cells that release the chemical transmitter acetylcholine.
Some researchers have also looked at stimulating a part of the brain called the ventral capsule/ventral striatum, which stimulates brain cells involved in higher-level cognitive functions like planning and thinking.
This all sounds very cool — but… does it work?
Researchers from the Leuven Brain Institute at the University of Leuven in Belgium published an analysis of all the data relating to DBS in Alzheimer’s — five studies published up until December 2021 — finding no significant evidence yet that the treatment is effective. The researchers of that analysis concluded that further gold-standard clinical trials will be needed to determine whether these treatments work. Other clinical trials are still in Phase 1 and Phase 2 of development.
“With DBS, we’re just trying to tap into the potentially
an abnormal circuit and augment it — not [to] reverse the disease, but more of [to reverse] the symptoms.”
Lee is optimistic about these early trials.
“The trials that have been looked at have shown promise,” he said. “We’ve started looking at DBS in patients already diagnosed with Alzheimer’s disease [in the early stages].”
Potential side effects
Two main types of risks/side effects occur with DBS. The first relates to the surgical procedure, as Lee explained, which runs the risk of infection and bleeding.
The other side effects may depend on where the DBS electrodes are placed in the brain. Lee added that research on more participants might be needed to tease out specific side effects. They haven’t seen any significant side effects so long as the electrodes are placed in the right spot. “We’re trying to target particular regions of the brain,” Lee said. “But if you stimulate regions of the brain that you don’t want, there can be side effects.”
How much does DBS cost for Alzheimer’s?
Currently, participating in clinical trials is the only way to receive DBS. If the FDA eventually approves it, experts estimate that the cost of DBS for Alzheimer’s will probably be similar to its cost for Parkinson’s disease.
Other types of neuromodulation for Alzheimer’s
Scientists are also developing new ways to stimulate the brain that are less invasive. There are some caveats to some of these techniques, however.
While DBS affects a very small, specific set of brain cells, Lee said other less invasive techniques are “less specific,” meaning a large group of brain cells is stimulated: “The question is whether or not that’s going to be effective at all,” he said.
The other potential problem is that less invasive methods don’t provide continuous 24-hour stimulation as DBS does — you only receive stimulation when using the device.
Nonetheless, these other forms of brain stimulation all show some promise in research and clinical trials.
Repetitive transcranial magnetic stimulation (rTMS)
Repetitive transcranial magnetic stimulation (rTMS) involves using a device that pulses magnetic fields to stimulate brain cells. The device can look like a handheld scalp massager or a cylindrical hair dryer helmet you might see at a salon. TMS is already being used for treating depression, but no device has been approved for use in Alzheimer’s yet.
In 2019, an FDA panel rejected a brain-stimulation device, Neuronix, that combines rTMS with cognitive training, which did not show positive results in its Phase 3 clinical trial for early Alzheimer’s disease. “There may be some value for TMS in cognitive therapy, but the current pivotal trial certainly didn’t demonstrate it,” said Dr. David Knopman, a voting member of the panel at the time.
Temporal interference stimulation
At Imperial College London, researchers are developing temporal interference stimulation. To do this, they stick some electrodes onto the scalp, attach them to wires, and start zapping the part of the brain responsible for memory, called the hippocampus, with two different electrical fields simultaneously.
A recent study published in Nature Neuroscience led by Dr. Nir Grossman at Imperial College London showed that this technique might provide a brain boost to healthy individuals and will soon be tested in people with Alzheimer’s.
Using light and sound stimulation
Cognito Therapeutics is testing a wearable medical device that delivers light and sound stimulation to stimulate synchronized brain activity called gamma oscillations. This is thought to enhance the brain’s immune system and help clear amyloid plaques.
The company presented data from its Phase 2 clinical trial at the 16th Annual Clinical Trials on Alzheimer’s Disease (CTAD) conference, which suggested that it could slow the decline of a person’s ability to do everyday tasks and may reduce overall brain shrinkage.










