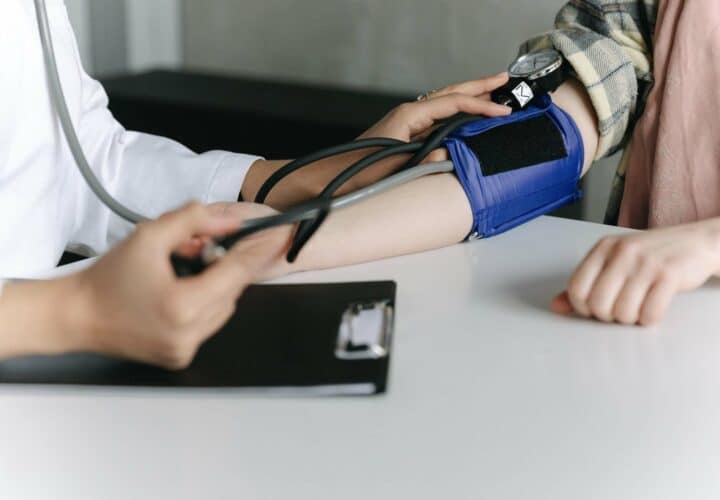
High blood pressure has been linked to both cognitive decline and dementia. Now, researchers are exploring whether drugs that lower your blood pressure could help treat or prevent cognitive decline.
As we age, we experience an increased risk of developing high blood pressure or hypertension — the leading risk factor for disease in the world. Dementia and cognitive decline are among the conditions for which hypertension increases the risk, and researchers are taking a closer look at this link.
Studies show that high blood pressure can damage the delicate blood vessels that support the brain, hindering their ability to carry oxygen and nutrients to different regions of the brain. Over time, this impacts brain function and cognition, sometimes leading to dementia.
To get hypertension under control, clinicians prescribe medicines that tell blood vessels to relax or that prevent them from constricting. Treating high blood pressure, some clinicians noticed an unexpected benefit: cognitive decline seemed to be kept at bay in some patients taking blood pressure-lowering medications. But curiously, not all of the patients showed improvements.
This observation builds on a wealth of research investigating links between blood pressure and dementia. An earlier study of 500 individuals found that high blood pressure, even at the age of 36, was a strong risk factor for dementia. Experts suggest that pathological changes in blood vessels are responsible for up to half of all cases of dementia.
Studies have also found that treating hypertension reduced the risk of cognitive impairment. Specific drugs that improve cardiovascular health, including statins and antihypertensives, were shown to reduce the risk of dementia by up to 21 percent.
Researchers from around the world collaborated learn more about the potential, publishing their findings in a meta-analysis in the journal Hypertension in June, 2021. The team looked at the effects of different blood pressure-lowering medications across people living in different countries, analyzing 14 trials with a combined 12,900 adults aged 50 or older across the U.S., Australia, Canada, Germany, Ireland, and Japan.
In addition, they asked: Do these medications prevent damage to blood vessels? Or do they affect the brain more directly?
What are the different kinds of blood pressure medications?
Although blood pressure medications work towards the same goal, there are several different kinds, and they operate in different ways. Each medication has a unique structure and properties that affect its distribution through the body. Some, but not all, of these medications make their way into the brain.
Among those that reach the brain are renin-angiotensin system drugs, including angiotensin-receptor blockers (ARBs) and ACE inhibitors (the ACE stands for “angiotensin converting enzyme”). The kidney releases renin, a protein that helps form angiotensin, into the blood. Then, ACE activates the angiotensin, which can then bind to sites on blood vessels, causing them to narrow. ARBs prevent angiotensin from sending its signal while ACE inhibitors prevent it from becoming active.
Other medications that treat high blood pressure do not cross into the brain. These include diuretics, beta-blockers, calcium channel blockers, alpha blockers, Alpha-2 Receptor Agonists, combined alpha and beta-blockers, central agonists, peripheral adrenergic inhibitors and vasodilators.
Treating high blood pressure means lowering risk of cognitive issues
What the researchers found is that a specific kind of blood pressure-lowering medication — the type that enters the brain and targets a system in the body called the renin-angiotensin system — appeared to reduce the incidence of new mild cognitive impairment cases by 19 percent. In other words, one in five MCI cases was prevented when renin-angiotensins were in use.
Further, the researchers found that adults taking renin-angiotensin medications had improved memory recall for up to three years, compared to those taking medications that did not get to the brain. This is despite having a higher risk for cognitive decline than individuals taking medications that do not reach the brain.
A co-author of the study, Jean K. Ho, a postdoctoral fellow at the University of California Irvine, summarized the findings for the American Heart Association: “It suggests that people who are being treated for hypertension may be protected from cognitive decline if they [are on] medications that cross the blood-brain barrier.”
The research continues
Despite the promising findings, there were some limitations. The researchers did not have enough information to account for racial and ethnic background in their study. Racial and ethnic minorities remain at a disproportionately high risk of hypertension and related disorders. They also respond and adhere differently to blood pressure medication.
Additionally, the proportion of men and women differed between the two groups. The study group which took medications that reached the brain had a higher proportion of men, who are already at a lower risk of dementia.
There are other ways to treat hypertension and boost your brain health, too
According to current guidelines from the American Heart Association and the American College of Cardiology, blood pressure-lowering medication may be prescribed when blood pressure reaches levels of 130/80 mm Hg. In addition to medications, changes to diet and exercise support a healthy circulatory system — and a healthy brain. For example, regularly eating a Mediterranean diet is associated with better physical and cognitive health.
Blood pressure-lowering medications will no doubt be more closely scrutinized. It is still unclear how they might interact with the brain to promote cognitive health. There is still so much we do not know about the mechanisms of dementia, but this study helps us uncover a new piece to the puzzle.