A few years ago, I had a minor heart attack. I had persistent soreness in my upper left back and, on a whim, I decided to check with Dr. Google to see what that pain could be signifying. Much to my surprise, the Google algorithm quickly returned the news that I was likely experiencing some form of cardiac arrest.
After a visit to urgent care, the emergency room and then a cardiologist, I was ordered to head directly to the cardiac wing of a local hospital. My memories of the few days in the hospital are somewhat fuzzy but I do know that either my husband Tim or sister Beth were there almost constantly, helping me navigate the new world of cardiac care.
I was reminded of those few days in the cardiac unit when I read an article in STAT News by Jason Karlawish, the co-director of the Memory Center at the University of Pennsylvania. In the article, Karlawish writes about his 83-year-old uncle who has Alzheimer’s.
“If he’s infected with COVID-19 and requires hospitalization, he’s in big trouble,” Karlawish said. “Smothering pneumonia can be deadly, but so can care in the hospital. One problem I can see right away is that his hospital will deny him a critical intervention: me.”
Hospitals and long-term care facilities have responded to the pandemic by banning visitors. We read heart-breaking stories about people dying alone, unable to be with family. I know I was certainly afraid when I was in the cardiac wing and can only imagine the fear that these people endure.
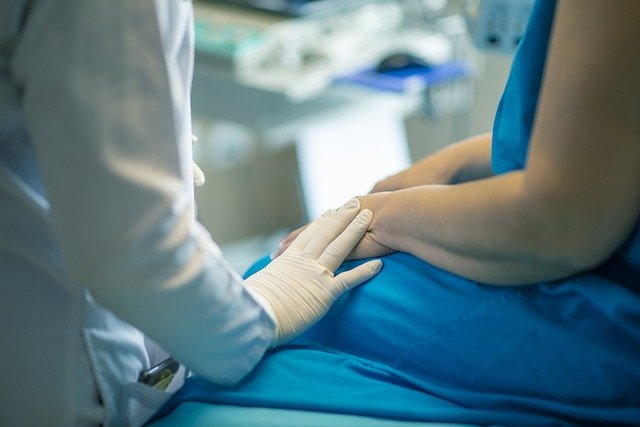
Above: Dr. Jason Karlawish discusses hospital delirium
and dementia in a Being Patient Brain Talk.
For people living with mild cognitive impairment (MCI) or Alzheimer’s, Karlawish says that the stakes are significantly higher than just fear alone. For those with Alzheimer’s, Karlawish says that a stay in the hospital can lead to delirium, which he describes as a “sudden onset of confusion and disordered thinking, a kind of acute brain failure.”
“Alertness waxes and wanes. Some people with it are lethargic. Others become fiercely agitated, tearing out catheters and intravenous lines,” Karlawish says. “Regardless of the response, delirium has a common feature: those who know the person well insist that he or she is really, really different.”
Karlawish experienced this first hand about a year ago when his uncle had a heart attack. “Within minutes of stepping foot in his hospital room,” he writes, “I sensed something was wrong. He was different. He was repeating himself, confusing me with my brother and asking what hotel this was.”
Ever since my diagnosis with early-onset Alzheimer’s a few years ago, I have been closely following all things Alzheimer’s. I served for a year on the Early-Stage Advisory Group for the national Alzheimer’s Association and am now on the board of the Delaware Valley Chapter. I’ve learned a tremendous amount about the disease but before reading Karlawish’s article, I’d never read about delirium and dementia.
In an interview, Karlawish told me it wasn’t surprising that I’d never heard the term. Until the late 1990s, he explained, doctors just believed that delirium was part of aging, much like how dementia was originally viewed.
“Finally people said ‘no, delirium is not just a part of aging,’” he told me. “And indeed the science was profound. There are certain things you do to older adults in the hospital that can increase their chance of getting delirium. And more importantly, there are things that you can do that reduce the chance of getting delirium.”
Karlawish says that as many as half of all cases of delirium can be prevented. “Prevention,’’ he says, “starts with people like me.”
“Patients with diminished cognitive abilities or trouble communicating need other people to be with them,” he writes. “A mother or father accompanying a hospitalized child is not simply a ‘visitor,’ they’re parents. The child needs a parent to help make decisions and provide reassurance and calmness—and so to heal.
“In the same vein,” Karlawish says, “I wasn’t visiting my uncle. I was his caregiver.”
That completely resonates. When I’m slipping into an episode, when suddenly the world isn’t making sense and panic starts to set in, a friendly face helps ground me and bring me back. Increasingly, I rely on my husband to see when I’m beginning to lose my grip on reality and to help redirect my thoughts.
Dr. Karlawish’s article proves, once again, that words matter. One person’s visitor is another’s critical caregiver. We will inevitably learn much from our national experience with COVID-19. I hope one of the enduring lessons will be a heightened understanding of the critical role that caregivers provide for people living with Alzheimer’s.
Finally, to wrap up my cardiac adventure, after a series of tests, the doctors pronounced me in good health and told me to go home, lose weight and work on controlling my blood pressure. They were never really able to tell me what had happened. My arteries were clear, my lungs clean as a whistle. Their best guess: a small piece of plaque had broken off and slightly damaged one of my ventricles and that’s why I was experiencing discomfort. One doctor later explained that I was lucky. “We thought you were really sick,” he says.
For more information about delirium, check out a recent report from AARP’s Global Council on Brain Health. You can also look up the Hospital Elder Life Program.
Phil Gutis is a former New York Times reporter and current Being Patient contributor who was diagnosed with early onset Alzheimer’s. This article is part of his Phil’s Journal series, chronicling his experience living with Alzheimer’s.