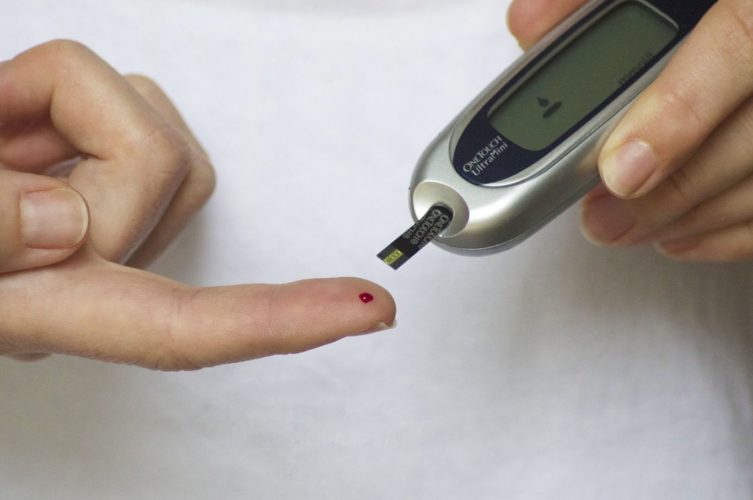
A growing body of research supports blood testing as a means for an accurate and affordable diagnostic test for Alzheimer’s, and a new technique may be the most effective version yet.
Blood tests for Alzheimer’s have been in development for some time, some of which have even been shown to have a 100 percent accuracy in diagnosing the disease. Some researchers have even taken the concept further, using artificial intelligence and machine learning algorithms to analyze blood samples and predict the progression of neurodegenerative diseases like Alzheimer’s. Most blood tests focus on the presence of specific genes which can produce RNA related to Alzheimer’s.
Blood biomarker tests were highlighted on Tuesday at the Alzheimer’s Association International Conference, the world’s largest gathering of dementia researchers. Maria Carrillo, the association’s chief science officer, said that “the possibility of early detection and being able to intervene with a treatment before significant damage to the brain from Alzheimer’s disease would be game changing for individuals, families and our healthcare system.”
Among the research presented at the conference was new work from Washington University School of Medicine in St. Louis, where scientists are searching for something new: p-tau-217. In a study published in the Journal of Experimental Medicine, a modified fragment of tau protein, p-tau-217 was found to accumulate in the cerebrospinal fluid of people with Alzheimer’s before the onset of symptoms, and also increases in levels as the disease progresses. The researchers, led by Dr. Randall Bateman, suspected they might find the same protein in the blood of people with Alzheimer’s, though likely at levels so low that they would be difficult to detect.
“We therefore wanted to quantify the levels of different tau proteins, especially p-tau-217, in the blood and compare them with amyloid pathology and onset of dementia to assess their potential as blood-based Alzheimer’s disease biomarkers,” explained Bateman in a press statement.
Bateman and his team developed a mass-spectrometry-based method capable of measuring the presence of p-tau-217 in samples of blood so small that they might contain only a trillionth of a gram of the protein.
“To our knowledge, this is the lowest concentration ever measured by mass spectrometry for a protein marker in human blood plasma,” said Dr. Nicholas Barthélemy, an assistant professor in Bateman’s lab.
The team found that, much like its presence in cerebrospinal fluid, levels of p-tau-217 are very low in participants without Alzheimer’s and elevated in participants with amyloid plaques, even those who had not yet developed cognitive symptoms. Results also indicated that p-tau-217 serves as a much more accurate biomarker for Alzheimer’s than p-tau-181, another protein previously proposed for blood testing.
Their findings further indicate that testing blood samples for p-tau-217 could allow for diagnoses years in advance of symptoms while being cheaper and less invasive than traditional PET scans and spinal taps.
“Our findings support the idea that tau isoforms in the blood are potentially useful for detecting and diagnosing Alzheimer’s disease pathology,” said Bateman. “Moreover, our assay for measuring plasma tau levels could be used as a highly sensitive screening tool to identify tau changes associated with amyloid plaque formation in normal subjects, replacing costly PET imaging.”
The Alzheimer’s Association’s Carrillo cautioned that the research on blood biomarkers is still early and it is not clear how long it will be before tests are available for clinical use.
“They need to be tested in long-term, large-scale studies such as Alzheimer’s clinical trials,” she said. “In addition, we need to continue research to refine and verify the tests that are the current state of the art — including cerebrospinal fluid and PET imaging biomarkers.”