A high percentage of care homes' residents in need receive basic care from family or unpaid caregivers, a new study finds.
With the ongoing pandemic, Vanessa Steil has been on pins and needles, hoping her 93-year-old grandmother’s care facility wouldn’t shut down visitation. Two days after her grandmother Marie Mongiardo moved into the nursing home’s subacute rehabilitation, in October 2021, the home placed a week-long visitor ban due to a positive COVID-19 case, Steil said. It was a difficult week for her and for Mongiardo, a two-time breast cancer survivor living with dementia. But Steil said she is thankful that, at the moment, she can safely visit and help provide care for Mongiardo, who is now in the home’s long-term care section.
“I call it caregiving 2.0 because … I’m there every single night to make sure she’s doing okay,” Steil, 35, who has been her grandmother’s caregiver for more than a decade, told Being Patient. “It’s hard. With dementia, she doesn’t really understand where she is, so I try to create some type of routine.”
The work of caregivers isn’t over when a loved one enters a nursing home or other care facilities. Often, they continue to provide routine care for residents, supplementing paid care. In fact, a recent study shows that, during pre-pandemic times, informal caregivers — family or any unpaid caregivers — provided an average of 37.4 hours of care monthly for residents in need at nursing homes, and those in residential care facilities received 65 hours of informal care monthly, on average.
Over the past two years, care homes have been devastated by COVID-19. Now, they are contending with the emergence of the Omicron variant. For safety, many facilities have mandated visitor bans and restrictions during the pandemic — with the unintended consequences of heightening residents’ social isolation and loneliness. Beyond these policies’ impact on residents’ psychological wellbeing, however, the recent study reaffirmed another repercussion of visitor bans, especially amid staffing shortages and burnout: the loss of informal caregivers who provide a considerable amount of basic care for residents.
“The bans essentially eliminated this invisible workforce, increasing the care demands on the staff, on top of the extra work of the COVID protocols and infections themselves,” the study’s authors Norma Coe and Rachel Werner of the University of Pennsylvania wrote in an article.
In an interview with Being Patient, Coe said it’s high time for acknowledging informal caregivers’ role in residents’ day-to-day care.
“Informal caregivers are providing a lot of care not just in the community, but they’re still providing a ton of care to people living in nursing homes and residential care facilities.” Coe, associate professor of medical ethics and health policy at UPenn, said. She added, “We need to really think about a long-term care policy that incorporates family members. We shouldn’t be treating them like free labor.”
In the study, published in Health Affairs, Coe and Werner analyzed data of two nationally representative surveys from 2015 and 2016. On average, they found that older adults who were in need and lived at home received 130.7 to 161 hours monthly of informal care; but those in nursing homes and residential care facilities still received an average of 37.4 hours and 65 hours of help monthly from informal caregivers, respectively.
Further, the researchers examined the type of help that older adults received. Among nursing home residents and those in residential care who required support with household activities, such as shopping and handling finances, the majority received help with these needs from informal caregivers. When it comes to mobility, like getting in and out of bed, most nursing home residents and about half of those in residential care in need were aided by informal caregivers.
For older adults who needed help with self-care, which included eating, bathing, dressing and toileting, again, the majority of nursing home residents received assistance from informal caregivers, whereas more than one in four older adults in residential care facilities received informal care for these tasks.
Meanwhile, the researchers pointed to one limitation of their study. “We can’t tell if this informal care is provided based on preferences of the elder and family members or due to needs of the residents being too great for the staff to meet alone,” Coe and Werner wrote. “If it is the latter, it raises concerns about adequacy of staffing levels in nursing homes.”
For Steil, herself a thyroid cancer survivor, she does the best she can to look after her grandmother alongside the nursing home’s staff — all the while working a full-time job and managing her own wellbeing. Monthly, she spends roughly 100 hours being a caregiver, Steil estimates.
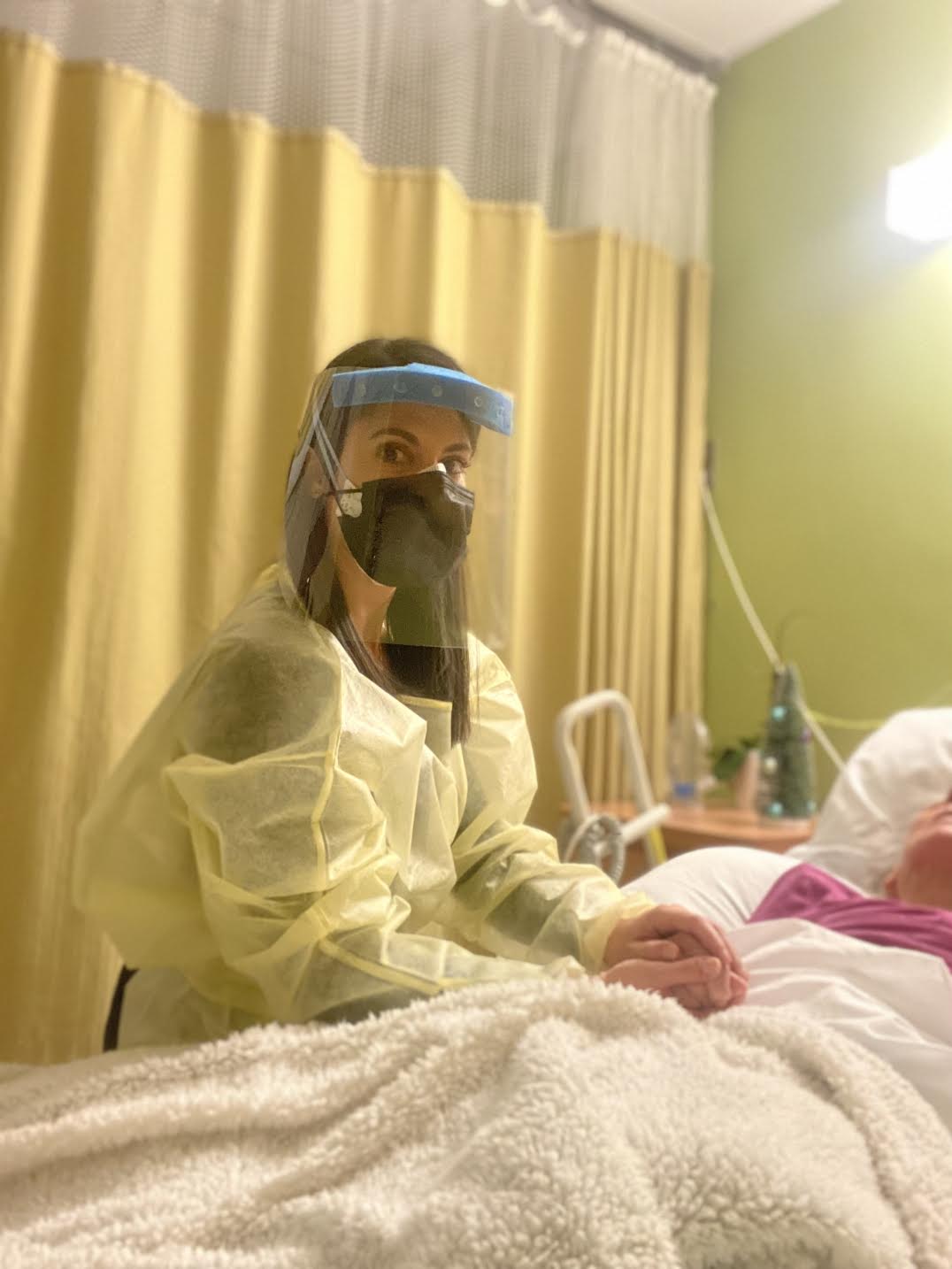
On the weekends, she finds time to manage Mongiardo’s property, finances and legal affairs. And every night, Steil dons a gown, a face shield, gloves and an N95 mask with a surgical mask layered over to accompany Mongiardo, helping her with dinner, monitoring her medications and making sure that she is warm and comfortable.
“She was very influential in raising me,” Steil, a board-certified patient advocate, said. “We have a special relationship and bond, so it’s important that I’m there.”




