Black Americans are two times more at risk of developing Alzheimer’s disease than non-hispanic white people. Why do clinical studies for cutting-edge new Alzheimer's treatments, diagnostics and preventions almost always have mostly white participants?
Experts estimate that, by 2023, nearly 40 percent of the more than eight million Americans living with Alzheimer’s and related dementias will be Latino or Black. But looking at trials that are underway and existing published research, Food & Drug Administration data shows that as of 2020, 75 percent of trial participants were white, while just 11 percent were Hispanic, 8 percent were Black, and 6 percent were Asian. Considering these latter populations have dramatically higher Alzheimer’s risk, one starts to wonder, why is Alzheimer’s research so white?
Image: Mollie Richards and Ralph Richards, Alzheimer’s advocates.
This disproportionately small focus on underrepresented communities in clinical trials for Alzheimer’s and dementia continues to have a huge impact on medical research from diagnostics to treatment, warn experts like Jason Resendez, executive director of UsAgainstAlzheimer’s Center for Brain Health Equity. And it’s creating a gap in understanding that is only just starting to be addressed.
Resendez and other experts in the field are trying to diversify research and learned what is driving this lack of diversity to begin with. Here are three of the biggest reasons they say clinical trials still fail to racially reflect the populations they are meant to help.
1. People of color can’t get involved due to limited information and barriers to access
Beyond just being more at risk of developing Alzheimer’s, Black and Latino communities are coupled with limited access to trial centers and the opportunity to participate in new research.
Resendez at UsAgainstAlzheimer’s spoke to Being Patient about this inequality. Many of these trials often take place at “ivory tower institutions who are serving their immediate community, which tend to be higher-resourced individuals who are predominantly white,” Resendez said.
Increasingly there is more work being done to build infrastructure beyond these institutions. Organizations like LatinosAgainstAlzheimer’s and AfricanAmericansAgainstAlzheimer’s are both increasing awareness and clinical trial participation among communities that are typically underrepresented.
This, advocates hope, will address barriers to access among minorities and empower policymakers with public health data on brain health inequalities.
2. People of color are hesitant to get involved due to a lack of trust in the research establishment
Resendez notes that, beyond geographic barriers to access, there is another big obstacle blocking Black and brown communities from participating in trials: These groups have a historically ingrained — and unfortunately, justified — lack of trust in biomedical research.
This distrust stems from hundreds of years of mistreatment in the medical community, the USPHS Untreated Syphilis Study being an infamous example. The study involved 600 Black men, 399 were living with syphilis. Participants’ informed consent was not collected and researchers told the men they were being treated for “bad blood.” On May 16, 1997, over fifty years after the study began in 1932, President Bill Clinton issued a formal Presidential Apology for the study.
Lack of trust, and unsuccessful efforts from researchers to rebuild this trust, has resulted in fewer participants from Black and brown communities in medical research and fewer brain donations.
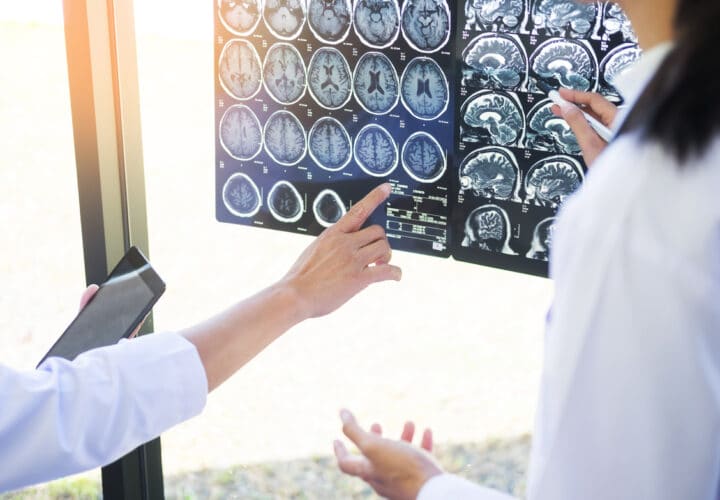
Despite advances in imaging technologies and scanning, a crucial component of breakthrough research in Alzheimer’s is researchers’ ability to study the brain after death. Researchers are experiencing this distrust first hand and are struggling to find donors from the Black community.
Shirley Fitch refused on behalf of her husband, Clarence, who passed away seven years after being diagnosed with dementia. She said the historical abuses of Black people in the medical field have been “awful and hard to get over.”
“I’m hesitant because of distrust,” Fitch told Being Patient. “Once my brain is donated for one purpose, who is to say it won’t be used for another purpose? It is out of your control.”
“They’re asking, ‘Do you care
about me? Are you here because
of research and the grants that
you’re making the money? Or do you
care about me and the community
and the people of color?”
Advocates are working to build trust back according to advocates Mollie and Ralph Richards.
Ralph Richards, a long-time Alzheimer’s educator and board member of Alzheimer’s Association Greater Indiana Chapter, told Being Patient how his work centers around rebuilding this trust through understanding cultural competencies.
In the couple’s community advocacy work, Mr. Richards said, they focus specifically on building trust and understanding cultural competencies.
“If you got to go in and talk to some African Americans, make sure that people that are going in and talking are also African American, or they’re not going to listen,” he said: This shows respect, he said, and it helps repair lost trust.
“They’re asking, ‘Do you care about me? Are you here because of research and the grants that you’re making the money? Or do you care about me and the community and the people of color?,’” he said. “If you can answer that question, then you have it.”
3. It’s on research institutions and drugmakers to build trust — and take accountability
Other experts including Caribbean neuroscientist Indira Turney agrees with the Richards family that having healthcare professionals of color can serve as an effective way to conduct outreach in African American and Latino communities.
Turney told Being Patient about her grandmother’s dementia diagnosis and how it inspired her to be an outreach leader in the Black community.
“No one is holding institutions
accountable for these low levels of
representation of people of
color in research.”
“I saw how much she deteriorated overtime, and also the effects on the family, just having to go through that process,” Turney said. “[I realized], I want to be a face that other Black and brown people can trust. I want to be a face that they can come to and say ‘You’re the one doing the research. So I trust you.’ Because the research needs to be done in our community, so we can know how to help each other.”
Poor outreach efforts to diversify research can be attributed to a general lack of accountability that has resulted in poor care for underserved communities.
“No one is holding institutions accountable for these low levels of representation of people of color in research,” Resendez told Being Patient.
”If there is no accountability, if there are no consequences for continuing business as usual with the lack of diversity, then it’s harder to change the status quo,” Resendez said. “It really takes having a commitment to wanting to do better science and being more ethical.”



The people from IBM are VERY smart and VERY educated. I am very hope full that after many tries the future will be much better than stopping with a person’s color… i mean ALL people should be !!