Dr. Eliezer Masliah explores the different biological targets of investigational Alzheimer's therapies.
Scientists know the physical changes in the brain that indicate Alzheimer’s disease happen decades before the life-altering symptoms take hold, thanks to detection techniques developed over the last ten years. Now that researchers think they know how a normal brain transforms into an Alzheimer’s brain, they can target specific genes and accumulations. At the top of their “most-wanted” list? Beta-amyloid, tau tangles, ApoE4, inflammation and vascular disease. We spoke to Dr. Eliezer Masliah, M.D., the director of the National Institutes of Health’s Division of Neuroscience, about what we can expect in the search for a cure over the next eight years.
- There are 20 to 30 new targets and genes that scientists have discovered that may be related to the development of Alzheimer’s
- We now have the ability to detect the signs of Alzheimer’s several years before symptoms kick in
- Some people accumulate protein plaques without developing Alzheimer’s, but the risk factor is how quickly they develop
Being Patient: There’s been this goal to find a cure by 2025. How feasible is that?
Dr. Masliah: I think there’s a very good chance. I’m very optimistic that considerable advances will be done by 2025. The question is, how do you measure that? At least in clinical development studies, we have what is called phases of clinical trials. It goes from phase one, which is more of a test of a drug safety to phase two, which is a smaller efficacy testing, to phase three, which is the ultimate test for a drug in a clinical trial. Right now in the Alzheimer’s field, we have several studies in phase three clinical trials.
“I’m very optimistic that considerable advances
will be done by 2025. The question is,
how do you measure that?”
Compared to other dementia disorders, Alzheimer’s clinical development is at a very high level. In the past 10 years, we’ve seen a number of phase three clinical trials in Alzheimer’s disease that have failed, but those trials are different from what people are doing now. If we look at basic science, it’s an explosion right now in Alzheimer’s disease. Originally, we only would talk about two targets, amyloid beta protein and tau. Now there are probably over 20 to 30 new genes and targets that have been discovered through the Alzheimer’s disease sequencing programs and other genetic studies.
Being Patient: Would something like inflammation be a target?
Dr. Masliah: We know a lot more than we knew before about inflammation. There are a number of genes involved in inflammatory responses. There are a number of these genes that are susceptibility genes for Alzheimer’s disease that have been discovered. I think we are experiencing a tremendous growth in the field.
Being Patient: What you’re saying right now is we’ve identified a lot of different factors that influence this disease or have an impact on it. We don’t necessarily know what the relationship is, but is it going to end up being an approach where you’re tackling a lot of these different things at one time, like we do in HIV?
Dr. Masliah: Yeah, I would say that—when we go to combinational therapy, where you’re going to have to attack the multiple targets simultaneously with two or three different types of drugs. At this point, we’re one step at a time. I think one of the targets that we’re looking into is amyloid beta. Another one is tau. ApoE is another important target. Inflammation is another target. I think as results start emerging in each of these individual targets, eventually some of them will start to be combined. Another one that we should mention is the vascular system.
Where’s Our Alzheimer’s Cure?
Karl Herrup on What’s Taking So Long
Being Patient: How much progress have we made in diagnosis?
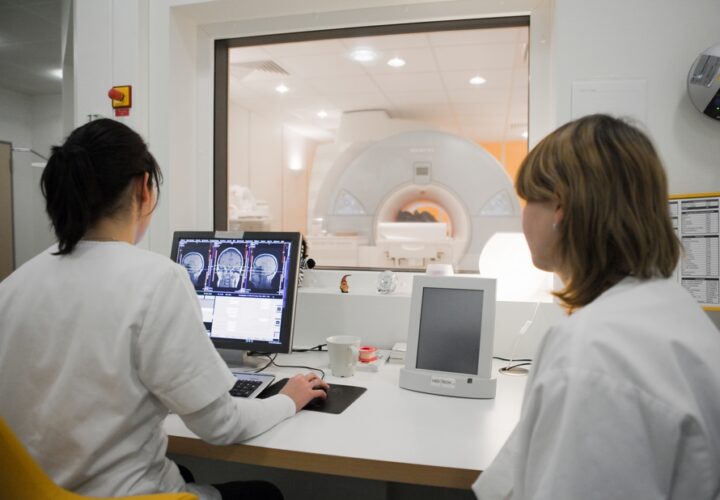
Dr. Masliah: Oh, that’s probably one of the areas where the most progress has occurred. I mean it’s absolutely a breakthrough what is happening in the past 10 years by developing both imaging techniques, like brain scans, to identify the amyloid and tau in the brain as well as biochemical or chemical studies in blood and cerebrospinal fluid for the early detection of Alzheimer’s disease. That, in combination with the genetic and the risk factors that we have now, means we can get the potential diagnosis of Alzheimer’s disease several years before the onset of dementia. That is really absolutely incredible what we have seen.
The only caveat there is that in those forms of Alzheimer’s disease that we call familial, where there is a genetic mutation that is causal of the disease, we can say with a very high level of confidence that that person will develop Alzheimer’s disease in the next 10, 20 years, et cetera. We also have the brain scans and fluid tests, but of course in those cases, the level of confidence that that individual will develop this disease in the next five to fifteen years, varies.
Being Patient: Aside from genetic predisposition, we think plaques and tangles indicate the pathology of this disease. But how do we know? There’s certain people who have plaque in their brain that never get Alzheimer’s, right? Or maybe they die before Alzheimer’s presents itself. Do we know the difference between the natural process of aging and actually declaring that these are hallmarks to the disease?
Dr. Masliah: There are now what we call longitudinal imaging studies, where the same individual is scanned for amyloid, tau, glucose metabolism or vascular disease. What we did before is we’d look at these people one time and try to say yes or no, but now we’re doing longitudinal scanning. What we can see is that the slope of the curve is very different. Those individuals, where there was a conversion from normal aging to Alzheimer’s disease, the slope as to how that amyloid or tau accumulated in the brain was much more faster than in those individuals that accumulated some amyloid in the brain, but never developed Alzheimer’s disease.
Detecting and Treating Alzheimer’s
Before Symptoms Set In, With Dr. Jason Karlawish
Likewise, one of the main or the main susceptibility genes for Alzheimer’s disease is this gene called ApoE4. Again, the slope is the same. It’s just that it’s earlier, the accumulation of that amyloid, with E4. Sure, as part of the normal aging process, you can accumulate amyloid and tau, but it’s really how rapidly, how early and what is the trajectory? What might predict if that person develops the disease? Again, let me just emphasize we can’t 100% guarantee that the person will get a diagnosis, unlike the familial forms like early onset.
Being Patient: If we’re getting better at diagnosing Alzheimer’s disease, what does that mean for taking us closer to a cure?
Dr. Masliah: It means that we can now develop clinical trials specifically targeting that protein or those proteins, utilizing those markers as the markers of the effectiveness of the therapeutics and that we have to go earlier and earlier in the disease. Everybody understands that if you detect cancer at a very, very early stage when the growth is limited, the chances of curing that cancer are much better than when they detect it when the cancer is spread throughout the body. Likewise, we’re able to detect Alzheimer’s disease before the onset of the clinical symptoms. The chance of the therapeutic to work is much better. It has not been shown yet, but that is the idea.


Very good focus on scientific research, but if attention and funds are not devoted to increasing Alzheimer’s clinical trial participation, there will not be persons living with the disease to test these new drugs. Currently less than 2% of those living with Alzheimer’s are participating in trials. 80% of trials are delayed and 30% never reach full enrollment. When the increased funds into research bear fruit in a few years, this problem will be great exacerbated. It would be great if Being Patient would do an article on the challenges of increasing clinical trial enrollment.
Indeed Jim, the subject of the ADRD clinical trial enrollment deficit needs more attention. We at BeingPatient are committed to helping bring more attention to this issue. In the meanwhile please see our article Will We Ever Find an Alzheimer’s Cure? The Answer Depends on Research Participants. Stay tuned for more on this topic. ~ Thank You.