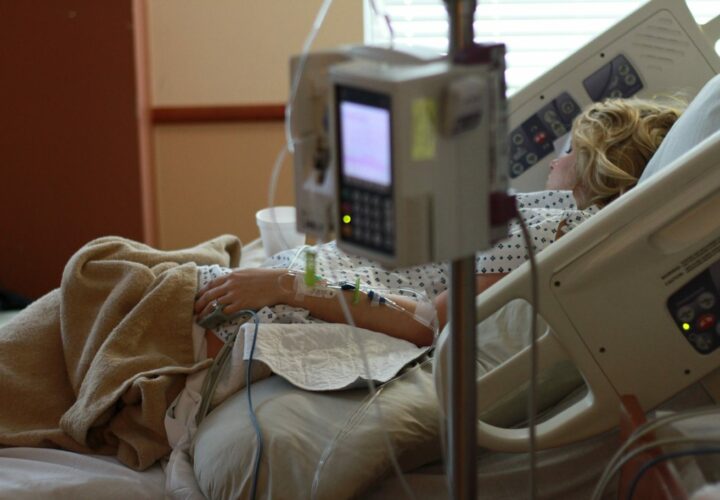
Antipsychotic drugs are most commonly used to treat mental health conditions like schizophrenia or bipolar disorder, but they’re also often prescribed to patients with Alzheimer’s or dementia to alleviate some of the most difficult symptoms.
However, this may come with some negative side effects: A new study finds that people with dementia who were using antipsychotic drugs were more likely to spend time in the hospital than those who weren’t on antipsychotics.
The study, conducted by researchers at the University of Eastern Finland, examined the use of two common antipsychotics, risperidone and quetiapine, over the course of two years. People using the drugs had, on average, experienced about 11 more days in the hospital compared to those not using them.
“Previous studies have not investigated the risk of hospitalization among persons with Alzheimer’s disease (AD) nor the accumulation of hospital days associated with antipsychotic use, although antipsychotics are commonly used in this group,” the authors wrote in the study.
Antipsychotics and Dementia
According to the Alzheimer’s Society, doctors prescribe antipsychotics, mainly risperidone, in cases of dementia to help treat behavioral and psychological issues. Risperidone is often prescribed in treating aggression in Alzheimer’s patients, and it’s typically used as a last resort, once non-drug pathways have been tried.
But doctors also have the license to prescribe other types of antipsychotic drugs for people with dementia, as long as they deem it appropriate, the Alzheimer’s Society notes.
However, antipsychotic use in dementia treatment has had a somewhat troubled past. One 2018 report found that nursing homes were misusing antipsychotics in an attempt to deal with disruptive behavior and symptoms among patients. The drugs have also been associated with severe side effects, including an increased risk of infections, falls, blood clots and stroke.
The latest study found that dementia patients who used antipsychotics were in the hospital for about 52 days on average, compared to 35 days for those who didn’t use the drugs. The researchers reported that hospitalizations among the patients using antipsychotics were caused mainly by mental and behavioral symptoms related to dementia, as well as respiratory, circulatory and infectious problems.
Though it’s unclear whether dementia patients using antipsychotics were more likely to spend time in the hospital because of adverse side effects from the drugs, the researchers note it’s important to take precautions when using or prescribing the drug for dementia patients given past concerns.
“These findings indicate the necessity for careful and regular monitoring of antipsychotic use to assess the response and decrease the risk of adverse events,” the authors wrote.



Risperidon is a very dangerous drug. It was given to my wife in 2015 when I put her into a clinic to improve her walking to calm her down because she did not feel at ease in the clinic which was a strange surrounding to her and I was no longer around, so she was probably upset. And like in many nursing homes, heavy chemical drugs are given to patients to calm them down. After giving Risperidon (without asking my agreement) for a week they had her calmed down, but she would not cooperate for walking improvement, so I took her home. However, after one week of Risperidon I did not recognize her anymore, she was without initiative, refused to get out of her bed for three days in a row. Spitex insisted that I continue Risperidon, because they appreciated how calm she was. But I stopped Risperidon and took her out of bed myself and built her up again into better condition. At that time she was also given Memantin against Dementia and I was told by a professor that the combination of both, Memantin and Risperidon can lead to death within 30 days… A specialised doctor from a psychiatric clinic confirmed that Risperidon is a very dangerous drug and should by no means be given to my wife and no calming drugs either. The peaceful environment at home and cared for by myself as her husband is the best treatment, as I told in my previous mail to you. Nursing homes and hospitals ruin the health of dementia patients with their chemical drugs, because they have only one goal: calm down the patients who do not feel at ease in that strange environment which they are not used to and are unable to adapt to it. If you have questions, please write.