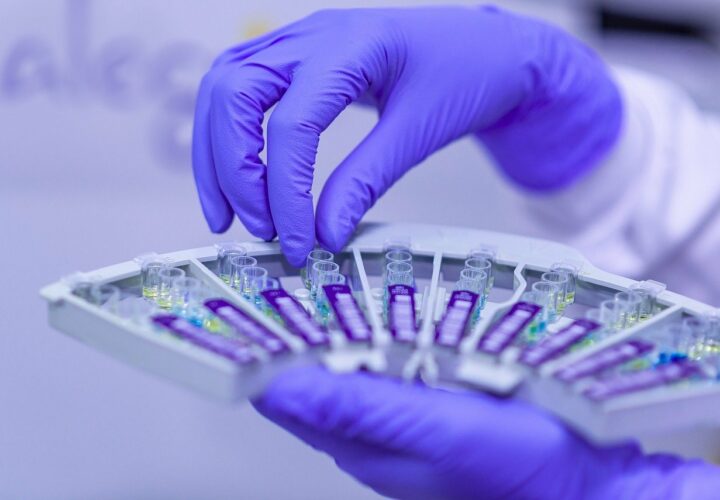
Cassava Sciences CEO Remi Barbier discusses the company’s Alzheimer’s drug candidate, simufilam.
Scientists are diversifying their approaches to finding an effective treatment for Alzheimer’s as clinical trials targeting beta-amyloid plaques, one of the hallmarks of the disease, have largely failed thus far. One of the experimental drugs that takes a different aim at the disease is simufilam developed by Cassava Sciences.
The company recently announced positive results of the drug in a Phase 2 study and plans to launch Phase 3 clinical trials in the second half of 2021. Being Patient sat down with Cassava Sciences President and CEO Remi Barbier to discuss the ins and outs of the research in simufilam and why Alzheimer’s is such a challenging disease to tackle. (UPDATE: Following that announcement and this talk, Cassava’s trial results have been called under scrutiny. The company has denied allegations of misconduct and fraud.)
- Simufilam targets misfolded forms of the protein known as filamin A, restoring their normal shape and function to counter neurodegeneration and neuroinflammation.
- In February, Cassava Sciences released initial results of the Phase 2 study of simufilam in 50 patients with mild to moderate Alzheimer’s. The company said the participants showed improved cognition and behavioral scores while showing no safety issues.
- In Phase 3 clinical trials, one study will enroll roughly 1,000 people with mild to moderate Alzheimer’s, who will be randomized to treatment with simufilam or placebo groups for an 18 month period. Another randomized, placebo-controlled study will involve a nine to 12 month treatment period of about 600 patients with mild to moderate disease.
Being Patient: What is Cassava’s approach to developing an effective treatment for Alzheimer’s?
Remi Barbier: Normally a drug aims to do one thing and only one thing. Our drug is a little bit different. We think of Alzheimer’s as multiple cascades. It’s not a single event. It’s multiple biological processes happening at once. It’s not quite a single waterfall. It’s more like Niagara Falls. You’ve got one big waterfall, but then you’ve got all these different waterfalls coming from the left and the right. Unfortunately, this is what happens in Alzheimer’s disease. It’s a series of cascades. None of them are good, and the outcome unfortunately is well known.
Our thesis is that if you go upstream of all of these different cascades, you’ve got a shot at not just fixing one waterfall, but a number of them. That’s been our basic hypothesis since we started working on our drug almost a dozen years ago.
Alzheimer’s truly is a mind boggling, complex disease. By the way, we’re not saying we understand it in more detail than anyone else. What we are saying is that we have some insights into the biology of the disease that are perhaps a little bit different from what others have been following. It’s that difference that I think results in the type of data that we’re seeing: the early evidence for improvement in cognition, the lack of any safety issues, the ability of our patients to tolerate our drug without severe side effects.
Being Patient: Can you tell us about the recent release of interim results of the Phase 2 clinical trial?
Remi Barbier: What we saw in an interim analysis of 50 patients on our drug for six months, in other words the halfway point, is an increase in cognition and a decrease in Alzheimer’s related behavior.
The good news is we just had a big meeting with the FDA in January. We just received the final official minutes of that meeting so now it’s official and they did give us the green light to move forward with a large pivotal Phase 3 program.
We plan to initiate those two Phase 3 studies in the second half of this year. Why the lag? Simply because it takes time. These are very large, complex studies and you just physically need drug supply, and you need a lot of clinical sites. It just takes a matter of months to get the organization and the drug supply up and running.
One study will be 1000 plus patients with mild to moderate Alzheimer’s disease. The second study will be shorter and smaller. It’ll be approximately 600 patients with mild to moderate Alzheimer’s disease. In order to thank the general public and the patients and the physicians, we do plan to offer open-labeled simufilam for those who complete the study.
We’re still actually putting together the list of what they call inclusion criteria, which is what you call the restriction. But typically the patients would be between the ages of perhaps 50 and 85. The group of patients that unfortunately we cannot help are those with severe Alzheimer’s disease. At that point, the damage is so far out that frankly I think it will be maybe a while before anyone can really help patients with severe Alzheimer’s.
Being Patient: What’s the target of your drug?
Remi Barbier: The target of our drug simufilam is a scaffolding protein called filamin A. We all have filamin A from your head down to your toes. That’s not the target. This specific target is an altered form of filament A. One of the contributions of our scientists and our academic advisors is that they made the unique discovery that patients who have Alzheimer’s disease have misfolded filamin A super early on.
Being Patient: Do we know if misfolded filamin A triggers the misfolding of beta-amyloid or the onset of Alzheimer’s?
Remi Barbier: We don’t know what day zero is and we certainly don’t know what causes day zero. But it’s well known by now that for patients who have the clinical symptoms of Alzheimer’s, typically the disease has been in place for a number of years. Whether it’s five years or 15 years, I don’t know. I don’t think anyone really knows.
But clearly, the germ has been seeded. The seed has been in place for many years beforehand. What we’re saying is part of that seed, if you will, is a misfold in this filament A. What our drug does is it sits on the filament A so that it is no longer distorted and shaped oddly. Our drug restores its normal function and shape.
Being Patient: What’s the difference between a disease-modifying therapy and symptomatic therapy?
Remi Barbier: Take the case of Aricept. I think we can all agree that you give Aricept to a patient with Alzheimer’s and initially the patient gets better. You get symptomatic improvement, the symptoms seem to go away. Unfortunately with Aricept, the symptoms come back with a vengeance. That is symptomatic relief. It’s almost like taking a painkiller when you’re in pain. You have a migraine or headache and you take the painkiller. The headache doesn’t really go away. It’s in the background but you can deal with it.
Symptomatic improvement is you make the headache go away. You hit something with the disease that modifies the actual disease itself. You’re no longer trying to put a bandaid on it. You’re trying to treat the underlying condition. That’s disease-modifying and that’s what we think our drug can do. Except we also know that because of what we’ve seen in early studies, we can both improve patients in the short-term as well as modify the course of the disease.
Being Patient: Have studies of simufilam measured biomarkers like beta-amyloid plaques and tau tangles?
Remi Barbier: We’re targeting neurodegeneration and neuroinflammation. Not one, not the other, [but] both. That makes all the difference in the world. In our early studies, we did require spinal tap, where essentially the physician goes in and takes out a very, very small quantity of what’s called cerebrospinal fluid. CSF is the fluid that runs up and down the spine. That’s necessary for a couple of reasons. One is you want to make sure that the drug actually reaches the intended target, and it does. We’ve measured that. But more importantly, we also want to see the drug’s effects on all these various biomarkers of disease with complicated names like neurofilament light chain, neurogranin, abeta42 (a form of beta-amyloid), ptau181 (a form of tau).
Essentially, all these are biomarkers of disease, biomarkers of inflammation. One thing we know for sure, with 100% certainty, is that if these biomarkers go in the up direction, cognition goes in the opposite direction.
We have a technique to bring down all of these biomarkers of disease. We think that by suppressing these biomarkers of disease, we’re targeting the underlying disease itself and we can actually improve cognition. If not improve, we can certainly stabilize cognition. That’s another point to consider: Stabilizing cognition is a huge win in Alzheimer’s disease. Why is it huge? Because we know with 100% certainty that cognition declines, typically by about four to six points on ADAS-Cog (Alzheimer’s Disease Assessment Scale – Cognitive Subscale). That’s one of the horrors of the disease.
For Phase 3, we will not require the spinal tap. There’ll be a small subset of patients [who will undergo spinal tap], but very small as a percentage of the total patient population.
Being Patient: Do you think multiple different treatments will be necessary to effectively treat Alzheimer’s?
Remi Barbier: I think it will end up more like HIV and perhaps other fields where once diagnosed, you will probably see the patient be given a cocktail of drugs, depending on the patient.
What biomarkers don’t predict with perhaps any accuracy is behavior. Behavior is a big part of Alzheimer’s disease. While we may be able to suppress some of these biomarkers — a lot of these biomarkers suppress neuroinflammation and make a real impact on disease progression — certain patients may still need for example an antidepressant or anti-psychosis medication. There will be room for many many different players. There will not be a silver bullet for Alzheimer’s disease.
There will be room for the anti-amyloid drugs. We’re certainly hoping that the Biogen drug (aducanumab) gets approved. We hope the FDA does the right thing, and provides it to patients. If so, our drug, with the Biogen drug and perhaps a number of other drug candidates out there, hopefully will make a difference in the lives of these patients, and these patients can have more good days than days.
Being Patient: Does the amyloid hypothesis still stand strong despite the many failures in drug development targeting beta-amyloid plaques?
Remi Barbier: Every patient with Alzheimer’s disease has amyloid plaque in his or her brain. But, not everyone with amyloid plaque in the brain has Alzheimer’s disease. How’s that for complications? This is why you can’t necessarily hang your hat on amyloid plaque and its removal. The anti-amyloid hypothesis definitely has a significant role to play in the overall science, but there has to be a little bit more to it.
Being Patient: Why is it taking scientists such a long time to develop an effective therapy for Alzheimer’s?
Remi Barbier: At the headline level, it’s just a hard problem. I’ll throw out a number: a trillion. A trillion is the number of cells that are estimated to be in the average brain, and you’re going in there and trying to fix maybe a small fraction of the trillion.
There’s just a lot of biology that we fundamentally do not understand. Understanding the brain may be one of the hardest problems at every level, not just at the level of biology but at the level of philosophy, theology, sociology, you name it.
Below that is there has been such a push to promote the anti-amyloid hypothesis. The anti-amyloid hypothesis is for real. It’s like climate change. It’s really hard to deny it. However, it may not be the final answer. It may not be the answer at all. We don’t know.
There’s more to it than the anti-amyloid hypothesis, which is not to say it’s wrong. It’s just that, like anything else having to do with biology, the reality is probably more complicated. We just need to expand our horizons around the types of innovations we’re willing to take on.
The interview has been edited for length and clarity.
Contact Nicholas Chan at nicholas@beingpatient.com