Lower levels of serotonin, the neurotransmitter that regulates happiness, sleep and appetite, may be a driving force behind the development of Alzheimer’s and memory loss, according to new research. A recent study by Johns Hopkins University adds weight to mounting evidence that low levels of serotonin are associated with Alzheimer’s disease.
How Does Serotonin Affect Alzheimer’s?
The question that scientists are trying to answer is what comes first: Are low serotonin levels what leads to Alzheimer’s, or do the changes in the brain that precede an Alzheimer’s diagnosis cause the serotonin levels to drop?
Participants with mild cognitive impairment had 38 percent less serotonin than their age-matched, brain-healthy counterparts in the control group.
While previous studies looked at levels of serotonin in people with Alzheimer’s disease, this study just looked at brain scans of people with mild cognitive impairment and memory problems.
Researchers looked at the brains of 28 adults with mild cognitive impairment who were an average of 66 years old and compared them to a group of 28 adults with cognitively normal, healthy brains of similar age and gender. Both groups underwent neuroimaging tests.
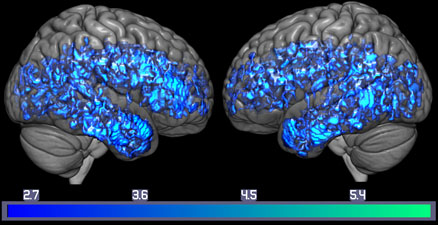
In the study, participants with mild cognitive impairment had 38 percent less serotonin than their age-matched, brain-healthy counterparts in the control group. They also performed 37 percent lower on verbal memory tests given in the study. Researchers say the association between memory loss and low serotonin levels suggests that serotonin may be a cause of the disease, rather than just being an effect.
What’s Next for Serotonin Levels and Alzheimer’s?
Research like this helps provide evidence for Alzheimer’s treatment drugs that aim to replenish serotonin levels, or to stop them from dropping in the first place.
“Now that we have more evidence that serotonin is a chemical that appears affected early in cognitive decline, we suspect that increasing serotonin function in the brain could prevent memory loss from getting worse and slow disease progression,” said Gwenn Smith, Ph.D., professor of psychiatry and behavioral sciences at the Johns Hopkins University School of Medicine and director of geriatric psychiatry and neuropsychiatry at Johns Hopkins University School of Medicine.
Lower levels of serotonin can significantly impact mood, especially when the levels are out of balance with other mood-controlling hormones like dopamine. Dipping serotonin levels are associated with depression, which is a risk factor for dementia. Symptoms of depression can lead to a more rapid cognitive decline.
Other studies have shown that low levels of serotonin are associated with more beta-amyloid, the toxic protein that forms into plaques in Alzheimer’s disease, in mouse brains.
A small dip in serotonin is a normal part of aging, but this study suggests that serotonin levels are affected in the earliest stages of the disease, when changes in the brain are present but clinical signs of Alzheimer’s, like memory problems and disorientation, are not yet present.
Along with lower serotonin levels, researchers also saw more gray matter atrophy and less blood flow in certain regions in the brains of MCI participants vs. the healthy brain group.
Scientists who worked on the study hope that serotonin levels might one day be used to flag people for dementia before clinical symptoms are present. That way, they may be able to make lifestyle changes that may delay further symptoms or enter a clinical trial that may be of benefit.


