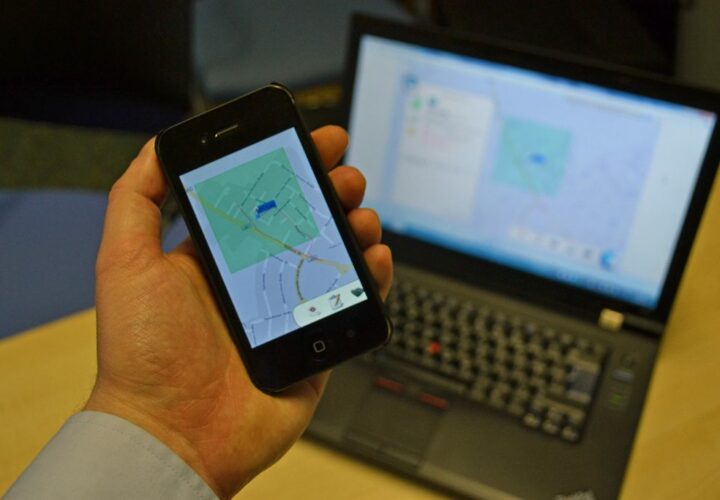
Being Patient explores both the benefits and limitations of assistive technology for the care of people living with dementia.
Eric Rosenthal’s wife, Eva, was diagnosed with dementia three years ago. While trying to adapt to the changes that came with her diagnosis, Rosenthal also struggled to find everyday technologies that could be adapted to fit his wife’s needs.
“I quickly realized that for someone with dementia, a smartphone isn’t so smart,” Rosenthal said. “Very early on, Eva would forget her code, didn’t know how to look up numbers and couldn’t even redial the last number. Then, she would lose her phone all the time, so between the complexity of the phone and finding the phone, I realized that the phone was not a solution for her.”

Rosenthal described the challenges he faced searching for technology that could help Eva to his daughter, Leda Rosenthal, a 19-year-old college student at Colgate University at the time. He said that during one of their conversations she said, “Dad, there’s got to be a better way,” and began researching assistive technology that could benefit her parents.
According to Rosenthal, Leda discovered that most caregivers have two problems when it comes to utilizing technology: They are not sure what issues they can solve with assistive technology and are unaware that there are products out there that can help them solve these issues.
Richard Fleming, a professor at the University of Wollongong in Australia and the executive director of Dementia Training Australia said that caregivers may be reluctant to search for assistive technology because they have enough difficulties already.
“The basic reason is lack of familiarity and an unwillingness to invest the energy in learning how to use new things at a time of stress and when energy levels are low,” Fleming said. “The situation will gradually improve as assistive technology devices, such as Google Home, become part of everyday life.”
Rosenthal thinks that although many caregiver chatrooms focus on caregivers’ emotions, few caregivers discuss tools they use that may improve their loved ones’ daily lives.
“They talk about problems like, ‘My loved one just became incontinent and I’m trying to deal with that. Any suggestions?’ or ‘They got lost and today was an awful day,’ but very few people have conversations about products they use,” Rosenthal said. “Everybody sends me to these emotionally-driven groups and what I need are some day-to-day solutions that are going to help me to be a better caregiver.”
Eventually, Rosenthal said Leda found that assistive technology is often more beneficial to caregivers than to dementia patients, since caregivers can use the technology with their loved ones, who may be too far advanced in the disease to find the technology helpful.
“That discovery was just a total game changer,” Rosenthal said.
Leda’s search for a ‘better way’ supports a recent study that was conducted at the University of Central Florida. The study found caregivers with loved ones in the early stages of dementia said their loved ones did not yet need assistive technology, while those with loved ones in the later stages of the disease said their loved ones could no longer use technology or required 24/7 care anyway.
Despite these findings, Pamela Wisniewski, lead author of the study and an assistant professor of computer science at the University of Central Florida, said that there are still ways technology can benefit caregivers with loved ones who have recently been diagnosed or are in the final stages of the disease.
“I think there are opportunities to introduce assistive technologies, especially in the early stages of Alzheimer’s, so that families can get used to the idea of integrating technology into their lives as the disease progresses,” she said. “In terms of very late stages, more invasive surveillance technologies, such as cameras and security systems, can help when the patient is less worried about their personal privacy and the caregiver needs to ensure their safety, even when they are in the next room. In some cases, surveillance technologies can give family members peace-of-mind when their loved one is in the care of a paid caregiver.”
Alzheimer’s Society in the U.K. is funding research on how to help people with dementia get the right information about assistive technology at the right time so that it’s easily accessible and they can remain independent for as long as possible, according to Lotty Davies, the research communications manager.
Davies said dementia patients themselves should have a say in product development.
“The development of assistive technology should include people with dementia in the design process to produce technological aids that are ‘fit for purpose’ without being too overly complex or requiring extensive training,” Davies said.
Wisniewski found that although most caregivers did not use technologies that were designed for dementia patients, they adapted common technologies such as home security systems or calendar applications to assist their loved one.
Similarly, Rosenthal said that although Leda found a lot of dementia-specific technologies exist, most of the technologies that he uses with Eva have not been created specifically for dementia patients and are everyday products that caregivers can repurpose. For instance, Rosenthal and Leda found that Amazon Echo was not useful to Eva when she used it by herself, but that it helped Rosenthal interact with Eva.
“At first, we thought, ‘Wow, this is really promising. Eva can just ask questions and the answer will come up.’ The problem was, she would forget it was even there in the middle of the table,” Rosenthal said. “But it was a really helpful resource for me because she would remember a song or ask a question and I would just say, ‘Alexa, play “Sgt. Pepper’s Lonely Hearts Club Band,” or ‘Just ask Alexa.’”
Through Leda’s research, Rosenthal found technologies that he now uses to assist his wife. For example, he purchased a “smart” pill bottle with a Bluetooth-enabled cap that connects to a cell phone and allows users to set reminders for when they want to take their medicine. While Eva cannot use the bottle by herself, Rosenthal uses it so that he can remember when to give Eva her medication.
The smart pill bottle is just one example of a series of smart devices that researchers are developing to assist dementia patients, including a smart dresser that could help dementia patients get dressed every day.
What Do Caregivers Think of Assistive Technology?
Through her research, Wisniewski also found that although some caregivers were reluctant to adopt assistive technology, most of them were interested in remote technologies that would allow them more freedom to leave their homes without having to worry about their loved ones.
The problem is that most caregivers don’t know where to begin. Caregivers in Wisniewski’s study said that the barriers to adopting these technologies, including the cost or lack of resources on how to find them, also outweighed any potential benefits.
There are various reasons why some caregivers may not be interested in using assistive technology, Angelo Makri, knowledge officer at Alzheimer’s Society, who specializes in wellbeing, said.
“They may be intimidated by new technology and think it might be a good idea in theory, but in practice feel worried about the learning curve that may be involved. Similarly, the person with dementia may be reluctant, and so the caregiver doesn’t want to mention it to them as they know it’ll lead to a difficult conversation,” he said. “Caregivers may also have difficulty knowing exactly where to look for products, and may not quite know what they are even looking for—so even if they know that a GPS or tracking device would probably be useful, they may not know which one would be best, if there are hidden costs, and so on.”
He said that generational gaps may cause some caregivers to not be as open to using new technology. He thinks caregivers may also feel guilty using assistive technology and as if they are taking away their loved one’s independence or infantilizing them.
Wisniewski said some of the caregivers in her study felt this way.
“Some participants referenced ‘Big Brother’ and other privacy concerns around the use of certain assistive technologies. While assistive technologies can be a solution for some families, it is important that all families feel comfortable with the level of technology being introduced to their homes,” Wisniewski said. “They should not be made to feel like they have to give up their personal privacy to ensure the physical safety of their loved ones.”
There’s also the question of whether fancy devices are worth the price when you have to think about the long-term costs of a dementia diagnosis.
“I tried $300 GPS innersoles for his shoes, but when I needed it, I had no cell service,” said Gail Schwartz Fellman, whose husband has dementia. “Plus, I did not have a clue when they needed charging so I tried as best I could to keep up. Had to pay $75 a quarter for service on top. I also had to swap them out, depending on what shoes he was wearing. Thus, it was a waste of money,” she said. “I am looking at getting an alarm for my front door so I will know when he decides to take a walk.”
Other caregivers reported that the technology their loved one used failed him or her.
“I used a great call device on his neck but my husband fell and never used it for four hours while he laid on the floor. [But it] might work in early stages and would be good if they wander, which he never did,” JoAnn Swenson said.
Fleming added that assistive technology should not be researchers’ only focus.
“My major concern is that we will put more resources and hope into the development of assistive technology support for people with dementia than we put into developing and supporting the human contact that people with dementia, like all of us, require,” he said.
Resources: Locating Useful Assistive Technology
Despite some setbacks, many caregivers believe that assistive technology could benefit their loved one.
After putting in so many hours finding solutions for her mother, Leda Rosenthal decided to use her research to help other caregivers, too. In 2016, she founded the company Alz You Need, a website to help caregivers find assistive technology. Leda launched the company through Colgate University’s Thought Into Action Entrepreneurship Institute after she received the 2016 Entrepreneurship Fund—competitive seed funding—to create the first version of Alz You Need.

Many of the mentors within the institute have told Leda that they believe she is doing something altruistic and that her tie to the disease makes her company meaningful, Rosenthal said.
While there are various websites dedicated to assisting dementia patients, Leda started the company because she felt there were no central resources that helped caregivers easily navigate the assistive technology that is out there.
The site allows caregivers to leave comments about products that are featured on the site, but they also plan on adding a forum where caregivers can share products they’re using or unique applications of existing products.
Because the Rosenthals realized that every caregiver has a different problem, they worked with specialists in the dementia industry to develop a free survey users who visit the site can take that assesses these problems and offers product suggestions that may provide a solution. As a matching service, the site recommends technology families think they may need and that they will feel comfortable using.
Since every family’s needs differ at various stages of the disease, the survey uses key details that assess each family’s ability to adopt new technologies, then creates personalized product recommendations. Alz You Need tracks over 150 companies and has a list of more than 40 standards that companies’ products must fit into to ensure that the site’s technology recommendations are comprehensive, up-to-date and that families do not have to spend time searching for products. The site organizes products into seven categories that range from “Cognitive engagement” and “Planning for the future” to “Health tracking” and “Safety.”
“We don’t want people to make any decisions. We just want them to answer a couple of questions about what their problems are and we’ll help them make the decisions,” Rosenthal said. “Most of us are not professional caregivers and we’re just trying to cope, not solve,” Rosenthal said.
While Alz You Need focuses exclusively on assistive technology that caregivers can use to help dementia patients, other organizations provide pages with assistive technology resources:
- Alzheimer’s Society in the U.K.: The page defines assistive technology, describes what assistive technology is out there, how to find the most practical solutions when searching for assistive technology and additional resources, including AT Dementia in the U.K., which provides information on assistive technology that can help dementia patients live more independently.
- Alzheimer’s Association: The pamphlet provides a list of research articles, product sites and apps that focus on assistive technology for dementia patients.
Alzheimer’s Society recently funded research into GPS trackers that can be placed into dementia patients’ slippers.
“Becoming lost and disoriented is a serious concern for people living with dementia and their loved ones—not only can it put them at risk of harm and stop them from being able to live independently, but it can also cause great stress to families and carers,” she said.
Makri said Alzheimer’s Society suggests that those who live in the U.K. can also contact their local Social Services department about products that they can get for free, rather than buying them privately.
What Types of Assistive Technology Are Caregivers Using?
In an informal social media poll, caregivers who use assistive technology said they found the following devices most useful:
Safety
- Baby monitors to track patients’ breathing
- Motion sensors to monitor patients’ movement
- Bed alarms to monitor when patients leave their bed
- Wireless door chimes to monitor when patients open doors
- Medical alert necklaces that caregivers or patients can wear, depending on what stage the dementia patient is in
- GPS trackers to manage wandering
- Tile item trackers to find your loved one, or missing items
- Home security systems with cameras to monitor patients
- Jitterbug phones to set up medication reminders, track patients’ locations and use the medical alert button
Cognitive Engagement and Memory
- Talking tiles to record reminders
- Voice-control virtual assistants
- Talking and atomic clocks
Health
- Fitness tracking apps
- Automatic locking pill dispensers to avoid missing or taking too much medication
The Future of Assistive Technology
Where is assistive technology headed?
Makri said there is a lot of interest in virtual assistants, such as Amazon’s Alexa, Apple’s Siri and Google’s assistant, so future research may focus on how those devices can best help someone with dementia.
“These virtual assistants can be great for people with dementia, not only in terms of helping them with daily tasks, reminders and so on, but also because they will answer the same questions repeatedly without sounding annoyed or agitated, ” Makri said. “Some of them can also be attached to home systems to control the lights, the thermostat, the curtains as well as other things.”
In addition to virtual assistants, Makri said there are also artificial intelligence program chatbots being developed which can talk to someone the same way a human would.
“At present, the chatbots are apparently not very good at all, but in time they may be indistinguishable from having a conversation with an actual person, which is as impressive as it is scary,” Makri said.
Wisniewski said that students in her lab are working on a mobile app called “Carebit,” based on the Fitbit API and step and heart rate tracking wristband, to help caregivers monitor their loved ones who are still living independently.
“The idea is to help prolong independent living but reduce the risk that an elderly or chronically ill loved one could become incapacitated, for example, going into a Diabetic coma, without someone checking in with them on a regular basis. Carebit provides hourly sign-of-life notifications that could potentially alert a loved one if a patient needs help,” Wisniewski said.
Fleming said advances in virtual reality are starting to show that people with dementia can have meaningful experiences by reliving past experiences, including driving a car or visiting somewhere from their childhood, facilitated by a virtual reality apparatus.
“Whether these virtual experiences can take the place of real experience and genuinely support a sense of meaningfulness in a person, remains to be seen. The same question applies to the provision of robots to comfort and amuse people with dementia,” he said.
Davies said that it’s important assistive technology is used for the right reasons: to enhance the independence, safety and daily living of a person with dementia.
“It mustn’t be used as a way for the carer to monitor a person with dementia without their consent. Assistive technologies should only ever be used alongside human interaction and not instead of it,” she said.