What is immunotherapy for Alzheimer's?
This article was produced by Being Patient in partnership with Charter Research. More information on Alzheimer’s clinical trials can be found on the Charter Research website.
Immunotherapy aims to prevent or treat a disease with drugs that stimulate an immune response. The success in immunotherapy for treating cancer and autoimmune diseases has led scientists and drug companies to explore its potential in treating people with Alzheimer’s disease. As clinical trials are now underway, Being Patient spoke with Dr. Jeffrey Norton, principal investigator at Charter Research and clinical trial participant Lynn Barnes, about the science behind the treatment and what it’s like to participate in a clinical trial.
- Immunotherapy is a drug therapy used to boost the immune system to fight disease, now being tested on Alzheimer’s patients
- The drug BAN2401 is an ongoing trial to target beta-amyloid plaques, a hallmark of Alzheimer’s
- Researchers are seeking to understand whether reducing beta-amyloid plaques in the brain can translate to meaningful clinical outcomes for patients
Being Patient: What does the drug BAN2401 do?
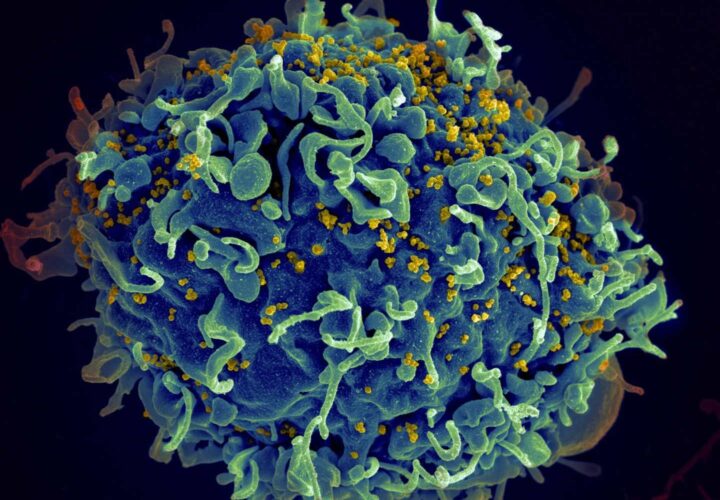
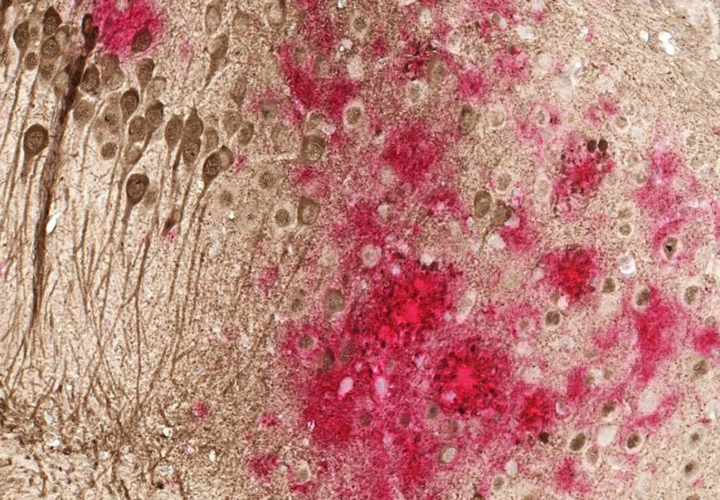
Dr. Jeffrey Norton: In memory impairment due to Alzheimer’s disease, the believed pathologic mechanism is the formation of abnormal plaques in the brain which are made up of a protein called amyloid, and also tau tangles, which is another form of tangled protein. We’ve actually known about the presence of these proteins for over 100 years. And Dr. Alzheimer himself, for whom the disease is named [after], first noticed this in a patient after [she] had died. During the last 100 years, we’ve been trying to understand where this comes from.
We’ve made a significant amount of progress. Now, we’ve gotten to the point where we actually have an antibody, which is an immune therapy, against amyloid. So it’s an anti-amyloid drug. It’s like taking some immunity from the outside of the body. Your body would then utilize that to block the formation of new amyloid and hopefully undo what’s already there.
Being Patient: Lynn, when did you first realize that you were experiencing memory loss?
Lynn Barnes: The best I can pinpoint is last year in October. I was sitting at the dining room table doing paperwork and I couldn’t put my thoughts together. It just didn’t seem right to me, and I kept talking to myself wondering what was going on. So I put the paper aside and came back [later] to do the work. And I just couldn’t understand what was going on. That is the one time, I can tell you, I realized something was wrong.
Dr. Jeffrey Norton: I want to commend her on being open minded and proactive, because I think all too often, what happens is people will ignore an episode like that … or they deny it, or their partner denies it.
Being Patient: Dr. Norton, what is the process of evaluating whether patients have Alzheimer’s or mild cognitive impairment, which may be due to the disease?
Dr. Jeffrey Norton: There’s a constellation of signs and symptoms, so the history that Lynn gives is very important — a change in your level of memory function. But then there are things such as a PET (positron emission tomography) scan, which she has had and which other patients have [had] — often in the setting of research — and many of these things can point in the direction.
Oftentimes, what we say is this person such as Lynn has mild cognitive impairment most likely due to Alzheimer’s, because at this point in time we can never say 100 percent. That being said, three out of four people who have dementia are going to have Alzheimer’s. And when you pair that with family history, it looks more and more as though [Alzheimer’s is] what’s going on.
Being Patient: What are the requirements for entering this trial?
Dr. Jeffrey Norton: There are lists of what are called inclusion and exclusion criteria. For this study, you have to be between the ages of 50 and [90], and you have to manifest symptoms like Lynn has described.
But it isn’t just that simple. There are fairly extensive cognitive tests. First of all, I think it’s important for people to know that all of the evaluation that you would get in participating in an Alzheimer’s disease trial is free of charge. The other thing is that you actually get evaluations that you can’t get even from a very sophisticated neurologist … Then, it includes things like PET scan [and] genetic testing. So you have to meet many criteria.
It’s a fairly rigorous process. A large number of people actually don’t get in for various reasons. They may have medical problems that are not allowed, or blood tests that don’t pass.
Being Patient: How far along the process is the drug?
Dr. Jeffrey Norton: BAN2401 is in phase three. That means it’s been through phases one and two. So this particular compound is far along in the process. This particular study that Lynn participates in has 1,500 people worldwide. And we’re looking specifically at mild cognitive impairment due to Alzheimer’s.
So this is proof of concept. We’ve now shown that in previous studies, it appears as though this agent does decrease plaque burden. But now, the concept is: does that translate to an improvement in overall clinical situation?
Being Patient: How long is the trial?
From the time you enroll until the time you finish, it’s 18 months. And the reason that this study is so long is there’s a six month [period] of what’s called extension phase. So the last six months of the study, every subject is actually getting what’s called the investigational product or drug.
That’s a little unusual for many studies. In most studies, neither the subject nor the investigator know if you’re getting what’s called a placebo, or the actual drug. So that’s one advantage to this particular study … About two thirds or more [subjects] have enrolled. We probably will be enrolling for a few more months but it’s hard to know. It depends on how many people qualify and it’s a little bit difficult to get in. But [it’s] absolutely worth trying.
Being Patient: Lynn, what’s it like to be in a clinical trial?
Lynn Barnes: I feel good that I’m doing something positive. And I keep my family informed with everything that I know. As far as doing it with this group of people in this study, I couldn’t have asked for a better support system.
I have a wonderful support partner in my study [who is] very knowledgable. And when I kind of fall through, she can just be there with me, talking me through it, and helping me figure out the right question to ask because I’m only one little brain here.
Being Patient: What motivated you to participate in the study?
Lynn Barnes: I feel like I’m a realist. I want to be able to give the most information I can to my family, to my husband. I have to say he’s definitely scared. The kids are scared. I understand that, but on the other hand, this is my life, and I need to do the best I can.
The interview has been edited for length and clarity.
Contact Nicholas Chan at nicholas@beingpatient.com