Can a simple eye exam detect Alzheimer’s disease? Researchers in Rhode Island and Florida have launched a $5 million study that could allow doctors to detect Alzheimer’s disease as early as 20 years before memory loss and other cognitive symptoms appear.
The 5-year study, called the Atlas of Retinal Imaging In Alzheimer’s Study or ARIAS, is designed to find structural changes in the retina that would allow doctors to identify and develop reliable and sensitive markers for Alzheimer’s disease.
Peter Snyder, a principal investigator for the study, explained that cells in our retinas are the same as the kinds of cells in our brains that are attacked by Alzheimer’s.
“Cell changes in the retina might reflect the same changes that are happening in the brain,” Snyder said in a news release. “We can look more easily in the retina to see the effects of the disease.”
Currently, the only way to identify a build up of amyloid protein associated with Alzheimer’s is through expensive PET scans that are rarely covered by insurance.
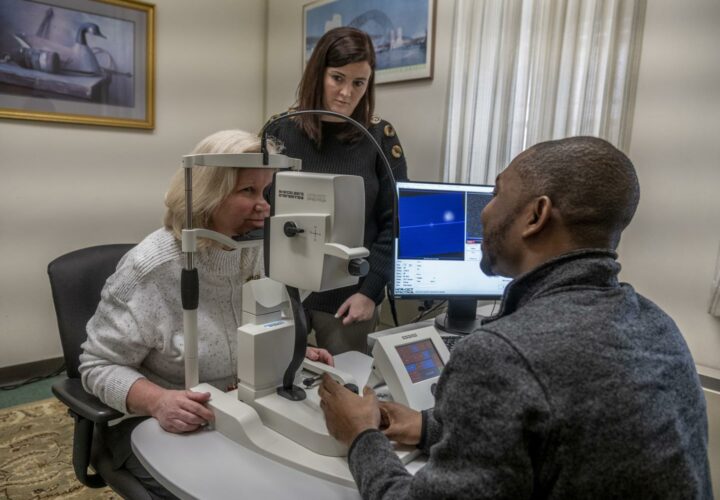
A special retinal scan, in contrast, would be relatively inexpensive and could be done by ophthalmologists during routine eye exams.
Snyder, vice president for research and economic development and professor of biomedical and pharmaceutical sciences at the University of Rhode Island, said that the research scans would take pictures of the retinas of participants with special blue, green and infrared lasers. These would allow for a microscopic level look at the anatomy, changes in pigment chemicals as well as the movement of red blood cells. The laser imaging technique would light up — or fluoresce — certain chemical pigments in the retina.
“We think atypical changes in the amount of these chemicals might signal high risk for Alzheimer’s disease,” he said.
The study is sponsored by BayCare Health System’s Morton Plant Hospital and St. Anthony’s Hospital Foundation in Pinellas County, Florida.
If the study is successful, researchers will identify a database of retinal changes that could serve as a “gold standard” to help identify risk for development of Alzheimer’s disease.
One of the ongoing challenges in research into finding a treatment or cure for Alzheimer’s is that identification and treatment typically only begins when patients are already symptomatic and when, most significantly, drug therapies may no longer be effective in slowing the disease in its earliest stages.
“When our study is completed, we want to make the technology available so that optometrists and ophthalmologists could screen for the retinal biomarkers we believe are associated with Alzheimer’s disease and watch them over time,” Snyder said.
“If clinicians see changes, they could refer their patients to specialists early on,” he added. “We believe this could significantly lower the cost of testing. We may then identify more people in the very earliest stage of the disease, and our drug therapies are likely to be more effective at that point and before decades of slow disease progression.”
Researchers are also exploring other ways of detecting Alzheimer’s before people become symptomatic. One possible venue are simple blood tests. In June 2019, for example, a study published in the journal JAMA Neurology found that a blood-based biomarker test called Elecsys correctly identified people with beta-amyloid plaques with 80 percent accuracy.
Early detection of Alzheimer’s and other dementias is not, however, without it challenges. Doctors and medical systems are now typically unable to provide much guidance for patients experiencing early memory or cognitive issues and new ways of early detection could make the problem much worse.
To improve how medical systems and doctors handle dementia, the Alzheimer’s Association this week announced a new program to improve dementia care in the clinical setting. Through the new initiative, the Association will work to engage more than 300 health systems across the country to improve health outcomes for people living with dementia.
“When dementia care is not managed well, or not at all, health outcomes are much worse and the costs are much higher,” said Joanne Pike, the Association’s chief program officer. “By working with health systems, we aim to improve both sides of the equation, where people living with dementia get timely, high-quality care and the cost to the system is lower.”
UPDATE, 20 November 2023: As of a landmark policy change in October 2023, Medicare now covers beta-amyloid PET scans for diagnosing Alzheimer’s disease.




Where can I get tested and is it covered by OHIP? If not, how much does it cost?
Joanne, this Eye Exam is in the research study stage. It is not available to the general public. ~ Thank you.
Tell me where to go. I live in Aventura, Florida. My husband has vascular dementia and is losing his speech though he speaks and comprehends frequently. How much is this test? He has Medicare and Blue Cross and Blue Shield. We need to do it now. Please advise.
Hello Erwin, this Eye Exam is not available to the general public. It is a research study at the moment. ~ Thank you.
My sister has Alzheimer’s. I would be happy to donate my time to this research.