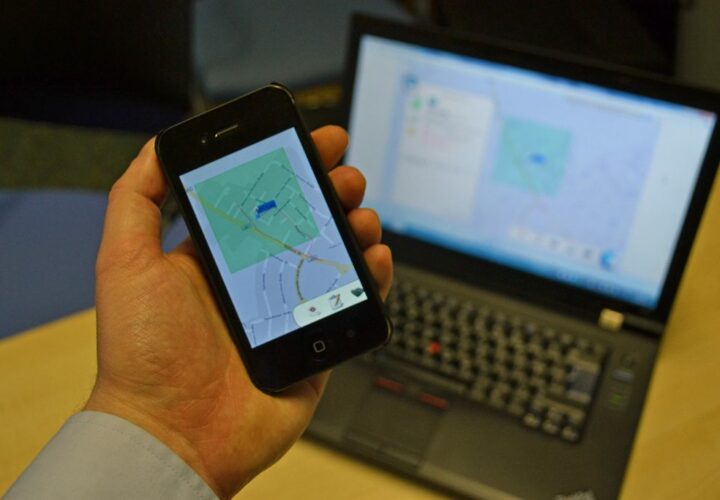
When people living with Alzheimer’s and related dementias wander or get lost, caregivers may turn to technology, local police, or their communities for help — or a combination of all three — but virtually no one can do it all on their own.
In June of 2016, the day after 73-year-old Jim Steele’s young grandkids spent the night, he went missing.
One of his grandchildren left their baby bunny in their crib, and Sherri Steele, Jim’s wife, went to run it down the block to their house in Texas. She was gone for only a few minutes, but when she got back, Jim was gone. There was no explanation, as far as she knew, for his disappearance.
“He’s very thoughtful and a very kind person. He wouldn’t just leave without saying that he was,” Sherri recalled. “He never allowed me to leave the house without telling him goodbye — it was as if we might not ever see each other again.”
After a few hours, she tried to track Jim’s phone, but after several attempts at calling him, she realized he had turned it off. At dark, she called the police. Two officers came to the house and asked if he had just needed a break from her, but Sherri knew his actions were out of character. She told them that she felt there was something wrong with him, but without a medical diagnosis of cognitive impairment, which Jim did not have, their hands were tied.
In most cases, if an older person goes missing, local law enforcement can issue a state-wide Silver Alert – a broadcast system that assists law enforcement in locating older adults, especially those with cognitive impairment.
Silver Alerts are issued on a state-by-state basis. Currently, 27 states have Silver Alert Programs. In the Steeles’ home state of Texas, documentation of a diagnosis is necessary to meet the Silver Alert criteria.
When Jim didn’t return the next day, Sherri looked at his credit card activity and found that he checked into a small hotel in a random town. The officers went to do a welfare check, but Jim had already left.
“Three days later he came back through the door like nothing had ever happened, with a bag of dog food in his hand, and he never knew where he went,” Sherri said. “He never discussed it. He seemed to be completely unaware that there was an event happening and that everyone was looking for him.”
That September, Jim was diagnosed with Alzheimer’s.
***
As of 2019, there were approximately 56,000 cases of missing adults pending in the FBI’s National Crime Information Center system. According to the Congressional Research Service, people living with dementia are at a higher risk as they may become confused and lose track of where they are.
Along with Jim, one of six people living with Alzheimer’s go missing at some point.
A study from the National Center for Biotechnology Information suggests that navigational difficulties can be a precursor to cognitive impairment diagnosis, as dementia damages the hippocampus, the part of the brain responsible for forming new memories specifically about time and location. This proved true to Sherri, as Jim and herself had moved to Washington State and were traveling back and forth to Texas, but she noticed that he did not know right from left, and could not follow the navigation system.
The Alzheimer’s Association recommends different ways to prevent wandering like a daily routine, activities during common occurrence times, reassurance, avoidance of busy or hectic areas, while also taking precautions such as hiding car keys, adding locks on doors out of sight and using technology to get alerts if a loved one leaves the house.
Whatever steps a caregiver may take or how watchful they may be, there will always be situations they could not plan for.
***
Elizabeth, another spouse to a person living with Alzheimer’s, uses technology to track her partner, 71-year-old Jane.
She utilizes Tile — a keychain that can be located within a 400 ft. bluetooth range and a loud ring in order to find missing keys, but while she is out, Jane utilizes Apple Maps on her own — one of the many technology tools that caregivers have turned to to help give them more oversight of people who wander. Other tech may include apps, like tracking app Life 360. Elizabeth’s system was a good one, but one day, things didn’t go according to plan.
One day near their home in Madison, Wisconsin Jane got lost when going to replace her watch battery, and Tile wasn’t going to be of any help — Jane had left her phone in the car.
She had forgotten where she had parked and, with her dogs whom she had brought along for the ride, she ended up walking for hours, making her way across a four-lane highway and eventually onto an unpopulated country road where she found a gas station to get water.
“The dogs are eight pound Yorkie mixes and they would never walk for almost eight hours and cover all of those miles,” Elizabeth said. “They were exhausted and as scared as she was, and I am still amazed they all survived.”
Elizabeth called the Madison Police, while her friends all began calling each other to see if anyone had seen her. In an attempt to find Jane’s location, Elizabeth and her friends used Tile and it showed her a neighborhood near a couple of their friends’ homes, shared it with police and met them there.
“Her car was parked on the street and their K9 officer was looking through the neighborhood; I had brought a sweatshirt of hers and some of our dog bedding,” Elizabeth said. “The officers were wonderful, compassionate and very thorough. We had been on that sidewalk for about half an hour when my phone rang, and it was Jane calling from a convenience store in another town about eight miles away – she had finally stopped and asked for help and they had let her use a phone.”
***
To help Elizabeth locate Jane, the Madison Police Department followed a standard that is followed by many departments across the country. They even have access to drone surveillance for rural areas, which would have assisted Jane if the search team deemed it necessary.
But protocols differ state to state and even local jurisdiction to jurisdiction.
All 50 states implement a Missing Persons Clearinghouse (MPC), which assists law enforcement in searches, recoveries and reunification practices to find “vulnerable adults.” While aiding law enforcement, the MPC offers “technical investigative assistance, referrals and advocacy in navigating the criminal justice system.”
“Along with Jim, one of six people living with Alzheimer’s go missing at some point.”
For example, the New York Police Department follows a patrol guide as to how to handle cases of missing persons, as well as utilizing their own MPC. For young children and elderly persons, the NYPD designates those cases as a special category missing, according to retired New York City Detective Investigator of 22 years, Victor Cabassa.
“The police get called, and a uniformed member of the police, or UMOS, determines that it is a special category missing, then notify the precinct level detectives,” Cabassa told Being Patient. “The detective shows up and asks for a bunch of information about the missing person: sex, mental capacity or memory.”
Cabassa added that when this basic interview is completed, the NYPD will use a level one mobilization, which is an alert or “Be-On-The-Lookout” (BOLO) sent out to the community. BOLOs are typically displayed throughout highways using signs similar to those indicating roadwork, lane changes, etc.
The search will typically continue for the next four or five hours, Cabassa said, and the police may use helicopters for surveillance, check in hospitals, check morgues, coffee shops or any other place the person could be.
“They spend the whole day sending troops,” Cabassa added. “If that fails, and only when that fails, then the precinct detective has another 24 hours of work on that case.”
The precinct level detective then refers the case to the missing persons unit, which then will assist the detective in tapping into different databases. This could lead to the installment of real time crime – using video surveillance, checking cameras or following bank statements.
“[People living with] Alzheimer’s usually go in the same direction, so we start that way, like checking the coffee shop two blocks away,” Cabassa said. “A lot of the time they end up simply in the hospital … as they were unable to express to the emergency medical personnel who they are.”
Smaller communities may have fewer resources. But they may have other advantages that can help balance the scales — like familiarity with the people in their communities.
***
When Neville Beaulah’s 84-year-old husband Donald, who is now in Memory Care, would go missing in Laurel, Maryland, her recourse would be to call the Laurel Police Department .
“In September of 2019, I’d learned by that point I [have to] immediately call the police,” Neville said. They found her husband time and again, and there was no wasted time at the start of the process, convincing them he hadn’t just left intentionally without letting her know… “He loved getting to ride in the police car,” she said.
Situations of a loved one going missing is difficult for any caregiver. Neville constantly worried about Donald taking off without saying anything.
Overall, there are many different types of responses available to families who deal with wandering or other missing incidents, such as using different tracking technologies, calling the police or utilizing community engagement. People rely on tech and local law enforcement, but caregivers are often relying on their community and their neighbors for help.
Organizations like the Alzheimer’s Association and the Missing Seniors Network try to make that community a little bigger. In Maryland, the National Alliance on Mental Illness (NAMI) offers a step-by-step guide to locating a loved one which follows similar protocols to that of the NYPD’s patrol guide.
According to the Alzheimer’s Association, if the police are not taking one’s concerns seriously, the Alzheimer’s Association 24/7 Helpline can help by speaking to law enforcement on a caregiver’s behalf to help secure a search. Meanwhile, the Missing Senior Network, a website that assists in sharing information and photos of someone who is missing, in order to allow for community members to aid in the search.
The job of a caregiver, especially a family caregiver, is a tremendous and difficult one, and during the COVID-19 pandemic, this task has only become more difficult.
“These days, lots of people feel out of control, and for good reason,” Dr. Steven Sabat, neuropsychologist and Professor Emeritus of Psychology at Georgetown University, told Being Patient in a recent interview about caregiving during the COVID-19 crisis. “There’s this thing going around, and you don’t know where it is, and you can’t see it. When we feel out of control, the anxiety levels go up. And so it’s really important to focus on what we can do, rather than what we can’t do.”
It may take some combination of technology, law enforcement and a village of support to navigate the recent uncharted waters. Experts say to seek out resources, remember that one human can only do so much, and don’t be afraid to ask for help.