The idea that a common viral or bacterial infection could lead, decades later, to the onset of Alzheimer’s was proposed over 30 years ago. The suggestion didn’t come out of the blue: As early as the 20th century, when Alzheimer’s disease was first identified and documented by German physician Alois Alzheimer, his contemporary Czech physician Oskar Fischer was already speculating about a possible link between the neurodegenerative condition and the bacterial infection tuberculosis.
For decades, University of Manchester biophysicist Ruth Itzhaki told Being Patient, the broader Alzheimer’s research community — and the entities that fund research — have been resistant to the idea that germs and dementia are linked.
But now, this “fringe theory” — as Nature Magazine put it in a look at the current state of the debate — is gaining traction.
Amyloid Analysis
The Amyloid Hypothesis proposes that sticky proteins called beta-amyloid peptides clump together in the brain, causing inflammation that then leads to neurodegeneration.
This theory has swallowed decades and billions of dollars in research, but increasingly in the past several years, people are wondering, “Is the leading theory about Alzheimer’s wrong?” Experimental Alzheimer’s therapies that target amyloid have continued to fail. This year alone, Lily and Roche canceled trials, and earlier this month, the Advisory Committee on Biogen’s experimental Alzheimer’s drug shocked everyone — trial participants included — by advising against FDA approval. Some researchers believe amyloid-target drugs are misguided and will continue to fail.
Whether or not the theory still holds promise, there is a call for a new approach to curing Alzheimer’s, and as the disease’s prevalence grows, that call is growing louder.
Infection Investigation
A November 2020 article in Nature discusses a number of microbes that could be to blame for the formation of Alzheimer’s – including a cause of lung infections (Chlamydia pneumoniae), the bacterium behind Lyme disease (Borrelia burgdorferi), the cause of Periodontitis also known as gum disease (Porphyromonas gingivalis), and the herpes viruses. However, Abbot writes that any infection, in theory, could trigger the overproduction of amyloid.
While the novel coronavirus pandemic has caused a notable surge in Alzheimer’s deaths since it reached the U.S. this spring, there is no evidence that COVID-19 may cause Alzheimer’s, but according to neurologists who have studied the impact of the Spanish Flu and other past epidemics on brain health, it is too early to tell. “We think that SARS-CoV-2 can reach the brain and it can stay dormant for many years and in fact, can contribute to memory loss, depression, psychosis, [obsessive compulsive disorder] and potentially Alzheimer’s disease,” Johns Hopkins University Affiliate Staff Dr. Majid Fotuhi told Being Patient in an interview earlier this year. It will be years if not decades, neurologists say, before there is definitive data.
As is usually the case in scientific research, the Infectious Theory has its fair share of criticisms that highlight key troublesome aspects of the concept. For the most part, the role of viruses in Alzheimer’s brains is studied via autopsy. However, Michael Heneka from the German Centre of Neurodegenerative Diseases believes that viruses could enter the brain during the last legs of life or perhaps after death, which could weaken the validity of post-mortem analysis.
Further opposition comes from Neuroscientist Bart de Strooper – director of the Dementia Research Institute at University College London – as he told Nature.com, “these studies [portraying the presence of infections in post-mortem Alzheimer’s brains] only show correlations which may have explanations that have nothing to with mechanisms.” He highlights the fact that noticing the mere presence of infection in Alzheimer’s brains does not imply their role in causing the disease.
The Amyloid and Infection Theories Converge
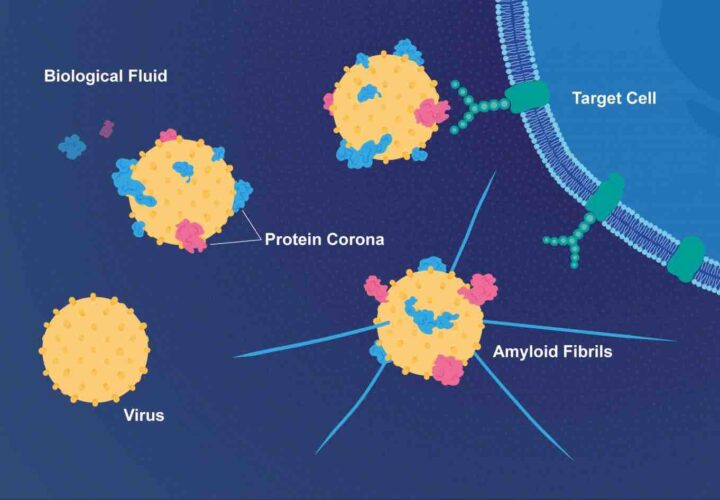
There is a world in which both theories are right. As Being Patient considered earlier this year, these two theories might not be inherently contradictory: Mounting research points to the possibility that amyloid, a key biomarker Alzheimer’s thus thought by many to be the cause, may actually form the villainous clumps in order to protect the brain from infection. However, the relationship between beta-amyloid clumps and Alzheimer’s is not so straightforward.
The Nature article discusses the research of both Rudolph Tanzi, a neurogeneticist at Massachusetts General Hospital, who found that the formation of amyloid plaques is a response to the presence of viruses, and who so named the theory the Antimicrobial Protection Hypothesis; and the research of Yueming Li, a chemical biologist at Memorial Sloan Kettering Cancer Center, who co-authored a study that found that when a virus enters the brain, a protein called IFITM3 activates and increases beta-amyloid production. This increase in beta-amyloid production grows more severe with age, corresponding neatly to Alzheimer’s.
However, the researchers are yet to find causation. Tanzi says that definitively observing the process of infection to amyloid response to Alzheimer’s, end to end, won’t come anytime soon: He told Nature, “We haven’t seen a smoking gun.”
Moving Forward
As the lives affected by Alzheimer’s disease continue to grow in number, so does the interest in studying the mechanisms behind it.
Two years ago, prompted by renewed research, Leslie Norins – immunologist and entrepreneur – offered $1 million to anyone who could prove the Infectious Theory. He believes that “the few pioneers who did look at microbes and published papers were ridiculed or ignored.”
With over 40 applications, the results of the race will be announced in March.
Heneka studies the immune system’s role in neurodegenerative diseases, and while he agrees that it is possible beta-amyloid forms in order to defend the brain from viruses, he says there is still far more work to be done: “I’ve talked to an editor recently from one of the top ten journals and she said the field is exploding,” Heneka told Being Patient. “And I told her: ‘With every explosion, there’s a lot of dust being generated and we have to wait until that is settled and see what good data remains.’”