Being Patient contributing editor and neurology researcher Simon Spichak did a deep dive into all the Alzheimer’s blood tests currently on the market. What he found: frustration, confusion, and a bit of absurdity.
Nothing is more exciting than when my favorite basketball team, the Toronto Raptors, announced that they were signing a star player that could help the team become really good. However, as it often turned out, the idea of this basketball player and the theoretical ways they would help the team seldom panned out.
Doing a deep dive into Alzheimer’s blood tests, I’ve found something similar: the idea of these tests is a lot more promising than how they’d end up performing in the real world. Often looking at the commercially available blood tests, I’d come away befuddled and sometimes catch myself yelling “What?” at my computer as I typed away. Here are the four takeaways from my reporting that I found strangest.
1. Alzheimer’s blood tests cannot actually diagnose Alzheimer’s
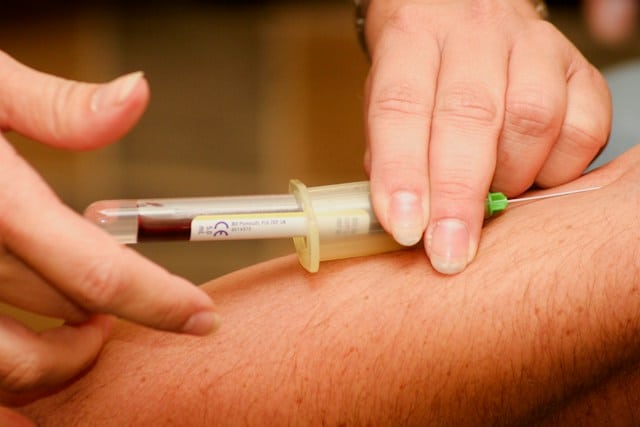
Right now, the gold-standard confirmation of an Alzheimer’s diagnosis requires a lumbar puncture or an amyloid PET scan. That isn’t changing with the new blood tests just yet.
The blood test results tell doctors whether someone likely has amyloid pathology in the brain that would be picked up by an amyloid PET scan. That information is used alongside a neurological examination and medical history to determine what exactly is causing a person’s symptoms.
If someone who is asymptomatic gets tested, it isn’t clear what the results will mean — especially since many healthy people develop beta-amyloid pathology in their brains, but never develop Alzheimer’s. Andreas Jeromin, chief scientific officer of ALZpath told Being Patient that the company intends to roll out their diagnostic test for asymptomatic individuals in the future.
This might change in the future, as scientists who are developing updated guidelines for Alzheimer’s disease are proposing a controversial change: People who receive a blood test indicating the presence of specific biomarkers could be considered to have preclinical Alzheimer’s disease — but only in a research setting.
2. These kinds of tests don’t receive FDA oversight in the same way drugs or other treatments do
In the U.S., the Food and Drug Administration is the gatekeeper for new drugs (like Leqembi) coming onto the market. Drug manufacturers must prove that their product is safe and effective before they can market and sell it. It isn’t perfect, and it’s been criticized by many Alzheimer’s researchers, but it does provide some standards and oversight.
There is some ambiguity for blood tests — many manufacturers classify their tests as “laboratory-developed tests” instead of “clinical diagnostic tools,” which allows them to skirt regulation. Unlike clinical diagnostic tools, laboratory-developed tests don’t currently need to prove that they are safe or effective or that their marketing is accurate. The laboratory that processes blood samples just needs to pass a basic inspection. (The FDA is looking to close this loophole and improve oversight in the future.)
Alzheimer’s blood tests, for the most part, are laboratory-developed tests that don’t need to prove they are effective. While some companies have used their blood tests in peer-reviewed published studies, others have not. There is simply a shallow barrier of entry for anyone that wants to make an Alzheimer’s blood test. It also means there is no guarantee that the results will be accurate or meaningful.
3. Alzheimer’s blood test biomarkers is a ‘Wild West’
Here’s a bit one: There are no universal standards for any of the biomarkers currently used by these various Alzheimer’s blood tests.
What’s that mean for patients? You can get your blood drawn and measure the levels of different protein biomarkers of Alzheimer’s disease. But it is nothing like testing for cholesterol or blood sugar levels, where there are agreed-upon and established cutoffs for determining your risk of having a certain disease. Each Alzheimer’s blood test company has its own threshold for what is considered a “positive” result.
Example: If the ratio of your Aꞵ42/40 proteins is 0.135, a test delivered by Quest Diagnostics would flag you as testing positive, while LabCorp’s ATN test would tell you that these levels are within a normal range.
“So yes, you can potentially take
six different Alzheimer’s tests and
receive lots of conflicting answers.”
For p-Tau181, things get downright absurd. Take LucentAD’s test considers a threshold of 14.2 pg/mL for the protein: If your levels are this high, then a doctor cannot rule out Alzheimer’s. But LabCorp’s ATN test considers anything above 0.97pg/mL higher than normal and a potential sign of Alzheimer’s.
So yes, you can potentially take six different Alzheimer’s tests and receive lots of conflicting answers! How are doctors supposed to interpret this information without these established cutoffs?
4. We have no idea how the tests will perform in the real world
Most of these blood tests have been tested in well-defined populations of patients in research studies and clinical trials. These research participants don’t have the same comorbidities as most people with Alzheimer’s — like high blood pressure, depression, diabetes, or heart disease.
We also know very little about how common medications influence the levels of Alzheimer’s biomarkers. One study showed that a common heart medication, Entresto, for example, can alter the levels of Aꞵ42/40, leading to a false positive result. That means in the real world, the actual accuracy of these blood tests might not be as high as in clinical trials.
We need more studies before we know for sure how effective and useful these tests are in the real world. After all, if a lot of patients take the test, even a false-positive rate of five percent could expose them to a number of undesirable outcomes, from unnecessary medical procedures and testing that are required to confirm an Alzheimer’s diagnosis, to damaging to their ability to secure long-term care insurance, to other impacts we haven’t even thought of yet.

Here’s another issue to add to the blood test confusion for ALZ. Dr. Dale Bredesen who is an ALZ researcher, physician and author. Dr. Bredesen believes that the amaloid plaques are PROTECTING the brain not the cause of ALZ. Please research this: Dale Bredesen Protocol
The End of Alzheimer’s – By Dr. Dale Bredesen
Apollo Health
https://www.apollohealthco.com › the-end-of-alzheimers
In his book The End Of Alzheimer’s, Dr. Bredesen unveils his groundbreaking protocol to prevent and reverse Alzheimer’s disease. The ..