Why to stop calling them "senior moments" — and how to tell the difference between these typical aging-related memory lapses and dementia.
Mild cognitive impairment (MCI), the condition associated with early stages of Alzheimer’s disease and related forms of dementia (like vascular dementia or Lewy Body dementia), can look a lot like “normal” aging. How can you tell the difference? According to the U.S. Centers for Disease Control, as of 2022, an estimated 6.5 million Americans age 65 and older are living with Alzheimer’s. Nearly three quarters of these Americans are in their 70s or older. As people age, cognitive lapses — like the occasional loss of a word or blanking on someone’s name in a conversation — are “normal” from time to time.
Being Patient talked to experts about the red flags that can help differentiate typical age-related cognitive changes from early signs of the cognitive decline which may be associated with neurodegenerative diseases like Alzheimer’s.
What is the difference between a so-called “senior moment” and dementia?
According to UCLA’s Sidell-Kagan Alzheimer’s Disease Treatment Development Program Director Dr. Sarah Kremen, people experiencing typical age-related cognitive changes can have difficulty retrieving information from the “rolodex” in their brains.
“This is common when people are trying to name something, either finding a word that they want to use, or frequently even [finding] proper nouns, which would include names of people or famous people,” Kremen told Being Patient in an interview.
That “tip-of-the-tongue” moment, when a person can’t seem to find the right word even though they know it’s somewhere in the back of their minds, might grow more frequent for older adults as they age.
After all, it takes longer for the aging brain to sort through information in the rolodex. With these “normal aging” memory lapses, the person will remember the words they were searching for eventually.
In the case of healthy aging, despite occasional forgetfulness, older adults will still form new memories, Kremen said. “They can remember what they did yesterday. They remember details of something they’ve read or conversations they’ve had. They can keep to their schedules. They can remember doctor’s appointments. They remember how to get to places.”
When these things stop being the case, however, it may be time for a closer look. But before going deeper, let’s address stereotypes around older adults and memory lapses.
Why we don’t love the term “senior moment”
There are all kinds of negative stereotypes society propagates about older adults. One of the most common is that older adults are forgetful, senile, and prone to what are very widely referred to as “senior moments.” One of the most frequently Googled questions about aging and cognitive health is “Is my senior moment the start of dementia?”
In fact, researchers are flagging that while cognitive ability does tend to decline with age, studies have shown that even the simple act of reminding older adults about ageist ideas and the “senior moment” stereotype can actually contribute to worsening memory problems.
“Older adults should be careful not to buy into negative stereotypes about aging — attributing every forgetful moment to getting older can actually worsen memory problems,” said Sarah Barber of the USC Davis School of Gerontology, lead author of the study. In fact, Barber’s team found, creating new positive stereotypes may actually be helpful to cogntive health aging.
“Our experiments suggest an easy intervention to eliminate the negative effects of stereotype threat on older adults — clinicians should simply change the test instructions to emphasize the importance of not making mistakes,” she said.
Now, back to looking at the cognitive decline typical of aging — and the cognitive symptoms that might mean something more serious.
So, when should you get cognitive testing for Alzheimer’s?
According to Kremen, people with mild cognitive impairment (MCI) — a clinical syndrome describing people who experience cognitive deficits noticeable to themselves or others that can be documented in objective cognitive testing — may have a hard time remembering details of their conversations just a day or the week before. They may have difficulty remembering appointments. Unlike before, they may need to write down reminders to keep track of normal daily tasks.
“Oftentimes, there’s a lot of misplacement of small items like keys, sunglasses or your phone, and not remembering where you put them down. There’s that constant search everyday to figure out where they were put,” she said.
While almost everyone has moments when they forget where they have placed an item, it’s a red flag when it happens nearly daily or weekly, intruding with one’s routine.
“What we hear when we talk to people’s families is that people may be repeating themselves,” Kremen said. “They don’t realize that in conversations, they’re telling the same stories.” Though others may be aware of their own repetitions. People with mild cognitive impairment may also ask the same questions.
Still, older adults with mild cognitive impairment can perform daily tasks such as working, driving, eating and showering independently.
“If I have mild cognitive impairment, does that mean I have Alzheimer’s?”
Older adults can have mild cognitive impairment due to Alzheimer’s, but people also suffer from the syndrome due to a host of other factors.
“There’s a lot of reasons why people have cognitive impairment,” Kremen said. “You can’t jump to the conclusion that ‘I have mild cognitive impairment, I must have Alzheimer’s disease.’”
For instance, people with obstructive sleep apnea, a condition when people’s breath stops for brief periods during sleep, can experience mild cognitive impairment. With proper treatment, clinicians can improve the cognitive abilities of these patients.
A review of people’s medication can also provide clues to the cause of older adults’ mild cognitive impairment. For one, Kremen said, medication for treating urinary incontinence can affect their cognition. Over-the-counter sleep medications, or the drug Ativan, commonly used to treat anxiety, may also lead to mild cognitive impairment.
Older adults with illnesses such as heart failure, urinary tract infection and thyroid problems can also have the syndrome, Kremen said. Clinicians can improve the cognitive abilities of patients with these conditions with appropriate treatment.
Does mild cognitive impairment automatically mean Alzheimer’s?
“Now on the flip side, if it is [due to] Alzheimer’s disease, then that’s important to know too obviously because that has an impact on the future of your life [and] your family’s life,” Kremen said.
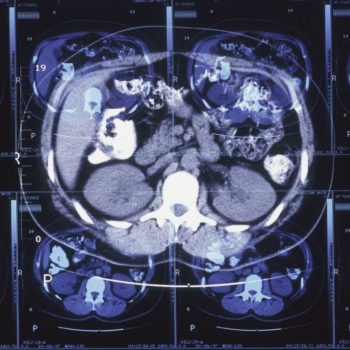
An FDG PET scan, which shows the patterns of metabolism in the brain, can help clinicians paint a better picture of whether the patient has mild cognitive impairment due to Alzheimer’s, Kremen said. Clinicians can also conduct a lumbar puncture, which involves drawing a patient’s cerebrospinal fluid to analyze levels of beta-amyloid and tau, biomarkers of Alzheimer’s. In addition, results from a battery of neurocognitive tests can also help clinicians stitch together pieces of the puzzle. To improve accuracy and accessibility of diagnostics for Alzheimer’s, scientists are developing tools like blood tests and retinal scans.
In general, Kremen said, clinicians in academic institutions have become more aggressive in determining the causes of mild cognitive impairment. That way, if they determine that the syndrome is due to a neurodegenerative disease like Alzheimer’s, they can begin managing people’s symptoms early on, and prepare patients and their families for care planning.
Can you stop, reverse or cure MCI?
According to Kremen, there’s currently no approved medication for mild cognitive impairment (MCI), and exactly how long it takes for the MCI caused by neurdegenerative disease — the progressive death of nerve cells in the brain — to bring about dementia symptoms varies from one patient to another. This said, research shows there are ways to protect and preserve your brain health and in some cases, slow down the progression of MCI or even reverse it, depending on its cause (sometimes MCI can be caused by hormonal imbalances, stress or other treatable factors).
There’s no way presently to reverse MCI caused by Alzheimer’s, but Kremen recommends her patients with mild cognitive impairment due to Alzheimer’s should exercise for 30 minutes a day, whether that is a workout or just an easy walk. Sticking to a healthy sleep routine and managing mental health is also important. Based on research, Kremen also advises her patients to eat a healthy diet that is low in saturated fat, consisting of fish with fatty acid like salmon, along with food with antioxidants like blueberries and cranberries.
“How can I tell if I have early-onset Alzheimer’s?”
A rarer version of the disease known as early onset Alzheimer’s (which is also known as younger onset) may make itself known at a much younger age. It is estimated to affect between 220,000 and 640,000 Americans. In people with early onset Alzheimer’s disease, symptoms typically emerge between the ages of 45 and 64.
For those concerned about the possibility of developing early onset, experts advise using the old standby of, “If you see something, say something.” If you see something amiss with your loved ones, experts recommend talking to a doctor, and considering cognitive testing. Because many doctors aren’t specially trained to spot early signs of Alzheimer’s, be persistent with your concerns.
Some of the main symptoms to look out for include forgetfulness and memory loss; language impairment; a loss of attention span; personality changes, mood swings, and social withdrawal. Learn more about those symptoms here and if you spot a few of them at once, talk to a doctor about getting cognitive testing.
Additional reporting by Nicholas Chan






my husband was diagnosed with MCI- being treated with a trial drug by lilly
improved memory. However, throughout this journey- he’s had weakness of his legs and sometimes balance and gait issues
Are these related?
Hello Susan, we suggest speaking with your husband’s doctor for a thorough evaluation. They can help determine if these symptoms are side effects of the medication, related to MCI, or indicative of another health condition that needs attention.
Here is an article you may find useful in the meantime on MCI: https://www.beingpatient.com/can-you-treat-stop-or-reverse-mild-cognitive-impairment-heres-what-the-science-says/