Subtle cognitive changes may actually precede the development of beta-amyloid protein in Alzheimer's disease, according to a new study.
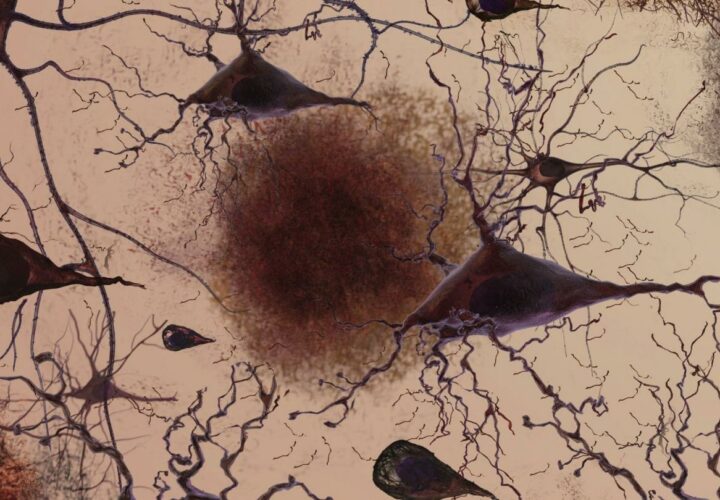
When it comes to Alzheimer’s, what happens first: beta amyloid plaques, or the visible personality and cognitive changes common with the disease? Researchers have long believed that amyloid drives neurodegeneration in the brain. But it’s possible that subtle changes in a person’s thinking abilities may actually precede the development of beta-amyloid protein, providing more clues to the complexity of the disease, according to a new study.
In the study, people with “objectively-defined subtle cognitive difficulties,” or Obj-SCD, were shown to develop amyloid in the brain faster than people who were deemed cognitively normal. It’s possible that being able to identify these cognitive changes earlier on with neuropsychological measures could help doctors identify when someone will be developing amyloid plaques in Alzheimer’s.
The study, published in Neurology, was conducted by researchers at the University of California (UC) San Diego School of Medicine and Veterans Affairs San Diego Healthcare System.
Neuropsychological measures to test Alzheimer’s cognitive changes
Because Alzheimer’s can’t officially be diagnosed until after death, during an autopsy, doctors currently use a variety of tools to help nudge them closer to a diagnosis when a person is alive. Those can include memory tests — which measure a person’s ability to remember things or use critical thinking skills — as well as neurological tests and MRIs.
But the earlier a person’s Alzheimer’s is identified, the better. And the new findings suggest that it may be possible to detect Alzheimer’s well before amyloid starts building up, and possibly even before any impairment on memory tests is shown.
By using sensitive neuropsychological measures — like how well someone is able to learn or retain new information — doctors may be able to get even closer to earlier detection. Early detection is key to getting patients the help they need to cope with, and possibly slow down, the progression of the disease.
“Prior work has likely used thinking and memory tests that are too crude to capture subtle cognitive changes,” Kelsey Thomas, assistant professor of psychiatry at UC San Diego School of Medicine and an author of the study, told MedPage Today.
In the past, researchers have explored other channels of identifying the disease before memory tests show any impairment — even through mobile games. In one study, researchers found that a person’s swiping, tapping and speed in games on their phones could hold clues to cognitive changes.
Further evidence to question amyloid hypothesis
The study followed 747 participants — 305 of whom were considered cognitively normal, 153 with Obj-SCD and 289 with mild cognitive impairment (MCI). The researchers measured the participants through neuropsychological testing, as well as PET and MRI scans.
The main takeaway was that among people with Obj-SCD, amyloid accumulation occurred much faster compared to those who were cognitively normal. People with Obj-SCD also showed thinning of the entorhinal cortex, which is a brain region associated with memory and time perception. Those with mild cognitive impairment, meanwhile, showed more amyloid at the beginning of the study — but didn’t develop it any faster than people with normal cognition.
“The scientific community has long thought that amyloid drives the neurodegeneration and cognitive impairment associated with Alzheimer’s disease,” Mark Bondi, professor of psychiatry at UC San Diego School of Medicine, said in a news release.
“These findings suggest that this is likely not the case for everyone and that sensitive neuropsychological measurement strategies capture subtle cognitive changes much earlier in the disease process than previously thought possible,” he added.
For years, researchers honed in on amyloid, believing it to be the main driver of cell death — and subsequent memory impairment — in people with Alzheimer’s. Known as the amyloid hypothesis, the idea was that if researchers target amyloid, in theory one could stop the progression of the disease.
However, setbacks among drugs and research targeting amyloid have led scientists to question the amyloid theory, and turn their attention to other factors that may drive the disease — like tau protein buildup or inflammation.
Ultimately, the researchers of the latest study hope that their results help doctors use other tools to identify the emergence of the disease even earlier — possibly before amyloid sets in.
“While the emergence of biomarkers of Alzheimer’s disease has revolutionized research and our understanding of how the disease progresses, many of these biomarkers continue to be highly expensive, inaccessible for clinical use or not available to those with certain medical conditions,” Thomas said in the news release.
“A method of identifying individuals at risk for progression to Alzheimer’s disease using neuropsychological measures has the potential to improve early detection in those who may otherwise not be eligible for more expensive or invasive screening,” she added.


So sorry to hear Biogen trial to cancellation for 5 million have this Alzheimer’s. People with heart disease have plenty of medication !!! You have worked on this Disease Since 1979 !!! Shame on you !!!!
Waiting for a cure ????
,