The study was in mice and the findings are still very preliminary, but researchers at Case Western University School of Medicine have identified a new previously unknown gene that could potentially be a target for slowing the advance of Alzheimer’s.
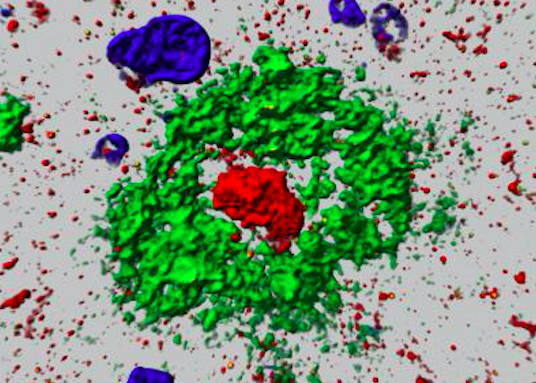
The researchers named the new protein “aggregatin” because it appears to accumulate — or aggregate — in plaque that develops in people with Alzheimer’s.
“Based on the data we have, this protein can be an unrecognized new risk factor for Alzheimer’s disease,” said Xinglong Wang, an associate professor of pathology at the university’s School of Medicine, in a news release. “We also see this as a potential novel therapeutic target for this devastating disease.”
The researchers published their findings in the journal Nature Communications. Their work was supported by grants from the National Institutes of Health and the Alzheimer’s Association.
The team has also filed for a patent for “novel Alzheimer’s disease treatments and diagnosis based on this and related study,” Wang said.
Aggregatin could play a role, the researchers said, in how a protein called beta-amyloid causes plaque formation that’s believed to trigger the atrophy that slowly destroys the brain.
While the relationship between amyloid and Alzheimer’s is well-established, the Case Western scientists said, less is known about how the protein actually turns into plaques.
That connection, Wang suggested, is where his team’s work appears to have broken new ground.
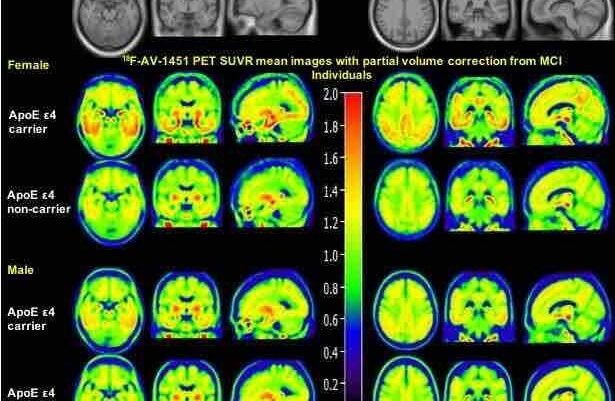
In the new work, the researchers began by correlating roughly a million genetic markers (called single-nucleotide polymorphisms, or SNPs) with brain images. They were able to identify a specific SNP in a gene linked to different patterns of regional brain atrophy known as FAM222.
Further experiments suggested that the protein encoded by gene FAM222A is not only associated with Alzheimer’s-related amyloid plaques and regional brain atrophy, but that aggregatin attaches to amyloid beta peptide — the major component of plaque — and facilitates the plaque formation.
When researchers injected mice with the aggregatin protein, plaque formation accelerated, resulting in more neuroinflammation and cognitive dysfunction.
Conversely, when they suppressed the protein, the plaques were reduced and neuroinflammation and cognitive impairment alleviated.
Wang said that proving his team’s initial findings would require additional research in humans and eventually would involve clinical trials with Alzheimer’s patients.
Another team of Case Western researchers made news in December when they said that an anti-AIDS drug called efavirenz could be modified to improve its ability to remove cholesterol in the brain.
Cholesterol, a waxy, fatty substance that’s most often associated with clogged arteries and heart disease, can also cause problems in the brain. Past research has found a link between cholesterol and beta-amyloid buildup in the brain, suggesting that cholesterol helps beta-amyloid stick together.