Xanax, Valium, Ativan and other benzodiazepines (“benzos”) are widely prescribed to treat anxiety in people living with dementia. But are they safe? Doctors weigh in.
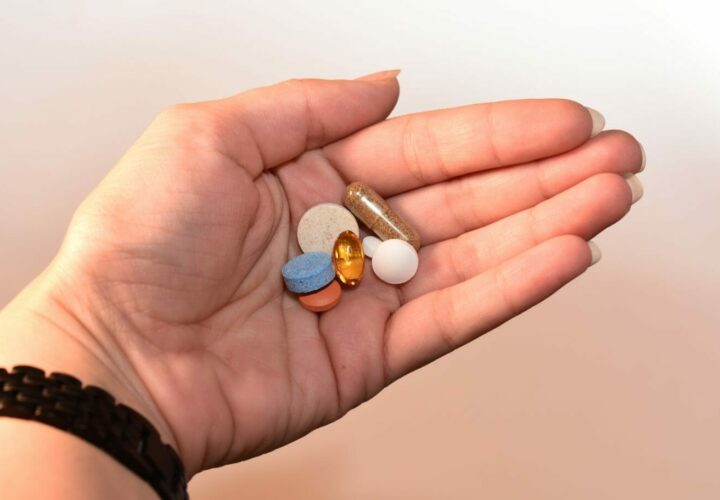
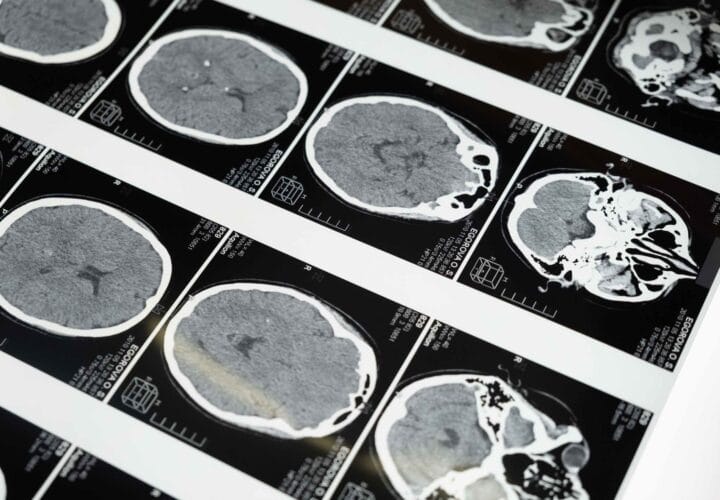
Dementia is most widely associated with its cognitive symptoms, like memory loss. But it often brings a host of behavioral symptoms, too, like agitation and sleep problems. In fact, as many as half of all people with dementia develop symptoms of agitation, which can lead to behaviors like pacing, restlessness, and aggression, both verbal and physical. Meanwhile, around one in four people with Alzheimer’s and other forms of dementia eventually develop sleep issues, like insomnia. To treat these conditions, doctors often look to sedative drugs like Xanax, Ativan and Valium. in the most commonly prescribed class of psychotriopics, called benzodiazepines.
Benzodiazepines come with substantial side effects and safety concerns — especially for older adults. And when they’re prescribed to people living with dementia, they’re being prescribed off label, as they haven’t been clinically trialed or FDA approved for this audience.
For these reasons, according to Dr. Paula A. Rochon, professor at the Women’s College Hospital, “benzos” are considered to be “potentially inappropriate for older adults and persons living with dementia.” She added that this class of drugs is considered potentially inappropriate for prescribing to older adult users in general, per European guidelines and the guidelines by the American Geriatrics Society.
According to Dr. Christina Reppas-Rindlisbacher, a clinician and PhD candidate at Women’s College Hospital could lead to emergency room visits, hospitalization and further loss of independence.
“Known risks of benzodiazepines for older persons include lethargy, increased confusion or delirium, increased risk of falls and fractures, and significant impairment of driving with increased crash risk,” Reppas-Rindlisbacher added.
Ultimately, it is up to doctors and patients to discuss the potential risks and benefits of benzodiazepines and any other medications before prescribing.
“The decision to prescribe any medication should involve a discussion between the patient and the clinician about risks and benefits,” Rochon said.
The first line of treatment is non-pharmacological
“Where possible, non-pharmacologic interventions such as reminiscence therapy and changes in environment should be tried first,” Rochon said. “Sometimes these symptoms are a response to an underlying medical condition, discomfort or unmet basic needs. As such, a comprehensive assessment by a dementia care team is invaluable to guide the development of a tailored management plan.”
Some of these risk-reducing environmental changes can include:
-
Removing tripping hazards and clutter
-
Rearranging the bedroom to provide more room to maneuver
-
Ensuring hallways are clear and well-lit
Other non-pharmacological ways to treat these symptoms include:
-
Reminiscence therapy which uses different images, sounds, smells, touch, and other modalities to help dementia patients recall parts of their memory.
-
Listening, dancing, or singing along to familiar music
-
Therapeutic interactions with real and robotic pets
Do benzodiazepines work better than other treatments?
According to the American Geriatrics Society, benzodiazepines aren’t recommended for people over 65 because they may increase the risk of falls, fractures, and hospital admissions related to these side effects.
For people living with dementia, there is also no strong evidence supporting benzodiazepines over other potential drugs like antipsychotics.
A 2014 study looked at all of the clinical trials of these medications conducted in patients with dementia. The authors concluded no support for the routine use of benzodiazepines. Compared to antipsychotics, they were less effective and had more side effects. Benzodiazepines may still be used when other treatments don’t work or have too many side effects for the patient to tolerate.
Treatments for agitation and insomnia in dementia
There are other classes of medications besides benzos that are often prescribed for treating agitation and insomnia. Some antipsychotics are prescribed off-label for treating agitation in patients with dementia, but they are also linked with increased rates of hospitalization among patients. Z-drugs meanwhile are prescribed for treating insomnia for dementia patients but could increase their risk of falls or fractures.
In addition, the FDA has approved some drugs specifically for treating these symptoms in Alzheimer’s disease.
FDA-approved treatments for agitation, insomnia and other symptoms in people living with dementia
In May 2023, the FDA approved Rexulti for treating agitation in people with Alzheimer’s dementia. The drug, which goes by the generic name brexpiprazole, is an antipsychotic initially developed for treating symptoms of clinical depression and schizophrenia.
In clinical trials, data showed that participants in the test cohort, who took the drug, showed more improvement in agitation over 12 weeks than the control group. However, the trial data also showed that the drug increased mortality from 0.3 percent to 0.9 percent. This is consistent with the known risks of antipsychotic medications when given to older patients.
Banner Sun Health Research Institute Director Dr. Pierre Tariot said that the results from the trial were a “major advance.”
“We had efficacy without all the toxicity that has plagued the other drugs we’ve been studying for agitation,” he said of studies on this class of treatment in dementia.
In 2020, the FDA approved Belsomra, a drug designed to treat sleep disturbances in Alzheimer’s dementia. Belsomra is also known by its generic name, suvorexant. In clinical trials, study participants in the test cohort, who took the drug for four weeks, slept on average 28 minutes longer than the control group receiving the placebo, according to the trial data.
Dementia, its symptoms and efficacy of treatments varies from case to case. If a loved one is taking a drug that isn’t working for them or that seems to have too many negative side effects, experts say caregivers should speak with their physician about changing the treatment strategy.
Rochon and Reppas-Rindlisbacher joined Being Patient EIC Deborah Kan in a Live Talk on benzodiazepines, why they are prescribed, and alternative treatments for people living with dementia. Watch the talk here or read a transcript below.
Q&A: According to Women’s Age Lab’s Dr. Paula Rochon and Dr. Christina Reppas-Rindlisbacher, who help patients and caregivers navigate decisions around medication, these drugs can come with significant side effects and safety concerns, especially for older adults living with dementia. The founding director of Women’s Age Lab in Toronto, Rochon is a geriatrician and senior scientist at Women’s College Hospital and ICES. Reppas-Rindlisbacher is a trainee with the Women’s Age Lab, working as a geriatrician while completing her PhD in clinical epidemiology and health care research at the University of Toronto.
Being Patient: First, talk about Benzodiazepines or “benzos.” We’re talking about a category of drugs like Valium and Ativan; people might be more familiar with Xanax. Can you tell us what these drugs are designed to do?
Christina Reppas-Rindlisbacher: I can take that question. This class of drugs, which we call benzodiazepines, and you gave them a very common example— thank you, Deborah. They’re designed to essentially slow brain activity. This is how they produce a drowsy effect, which is why they’re sometimes used to treat conditions like insomnia or panic attacks.
We’ll get into some of the side effects later, but I do want to mention up front that the use of these drugs can become problematic because the brain does get used to that slowing down effect and that drowsy effect that can lead to some drug dependence. This is why they’re listed as potentially inappropriate drugs to prescribe to older people, which, again, is something we can get into later, but in general, they slow down brain activity, which is just how they work.
Being Patient: Is it true that there have not been any studies on the use of these drugs on people with dementia?
Paula Rochon: In general, there’s been an issue of the kinds of drugs that older people tend to use [that] have not necessarily been tested on them in a way that we would like. Ideally, you want to make sure that if drugs are going to be used by a certain group of people in the population, that they were also included in those studies.
One of the issues that’s been in place for quite a while is that it wasn’t until a number of years ago that it was women that needed to be included in trials, for example, that were federally funded in the United States. Then, [it was] not till just a couple of years ago that older adults also needed to be included in trials that were funded by federal agencies in the United States.
So, you can imagine that older people, especially women, were not as perhaps represented as they should have been in these trials. As a result of that, for a series of different drugs, we don’t always have them optimized the way we would like for that population. That’s been a bit of an ongoing challenge.
“So, you can imagine that older people, especially women, were not as perhaps represented as they should have been in these trials”
Being Patient: Do we know that women are more susceptible to side effects than men? Is there any research in terms of the side effects?
Rochon: Well, one of the things that we do know, and then I’ll hand it over to Dr. Reppas to talk about this, is, in general, older people may be more susceptible, but women are particularly thought to be susceptible to adverse drug events.
Reppas-Rindlisbacher: The reason that women, and particularly older women, are more susceptible relates to the differences in how drugs are broken down. Women tend to metabolize or break down drugs differently than men, and as you get older, the way that you break drugs down also changes. Because of that, some of the side effects are some of the byproducts of these drugs that build up, [and] end up having a stronger effect in women and in older people. So, this is why we need to be particularly careful when prescribing drugs to these groups.
Being Patient: I feel like we hear a lot about benzodiazepines a lot. Do you know how often these drugs are prescribed for dementia agitation?
Reppas-Rindlisbacher: This is from my practice as a geriatrician, seeing older adults that have dementia. I would say they’re not the most frequently prescribed drugs. I know we hear about them a lot, but there are other drugs, I think, that are more frequently prescribed to treat some of the neuropsychiatric symptoms of dementia.
I think because benzodiazepines have many side effects, we hear about them a lot. But there are other drugs that are more commonly used, and typically, benzodiazepines are not. They shouldn’t be used first-line.
“I think because benzodiazepines have many side effects, we hear about them a lot.”
Being Patient: What is the difference between benzodiazepines and SSRIs, which are antidepressants, right? Is there a big difference in terms of side effects between “benzos” and SSRIs?
Reppas-Rindlisbacher: That’s a great question and a question we get from families and caregivers all the time. So, SSRIs, as you correctly said, are probably the most commonly used antidepressant to treat anxiety and depression across all age groups. They work by increasing serotonin in the brain, so they don’t have the same drowsy effect that benzodiazepines have.
They can be useful in managing some of the agitation and paranoia in patients with dementia because sometimes those behaviors are driven by an underlying mood disorder that either hasn’t been diagnosed or is really verbalized. So, I would say that, in general, these drugs are probably better tolerated.
They also have better evidence. Dr. Rochon mentioned that there’s not great evidence for any drugs, really, in the treatment of dementia, but the evidence that we do have points to SSRIs being well tolerated and having benefits in reducing agitation and caregiver distress. That’s why, if you’re going to use a pharmacologic treatment, we tend to prefer those drugs over the benzodiazepines. Many of the societies and the criteria that list adverse drugs, also make that recommendation.
Rochon: I think that’s a very good point. There are criteria. There are pieces out there to guide clinicians in selecting medications. One of the the guidance that people use is the BEERS criteria, especially in the United States, which is a really an explicit list of medications that are potentially inappropriate for use in older adults and drugs. Like for example, benzodiazepines are potentially inappropriate medications for use. So, there are lists that give some guidance in that.
Being Patient: So, benzodiazepines are on that list, as not recommended for older adults?
Rochon: Yeah, that category is potentially inappropriate medications. So, these are drugs where you want to think about other alternatives. Nothing is absolute, you know. I think when you think about things that are potentially inappropriate, there may be circumstances where you’re working with the family, working with your clinician, it’s decided that’s what you need to do. But for the vast majority of cases, they’re considered to be potentially inappropriate.
Being Patient: We have a question from our audience. She says she’s the caregiver of her sister with intellectual disability and severe cognitive decline. Her sister has been on Clonazepam and she was told to increase it for her aggression, but her sister has a flat affect, is tired and still aggressive because she thinks she’s tired from the med. She asks, are there natural alternatives or a “happy pill” out there? What are the alternatives to medications to manage behaviors that people with cognitive decline are experiencing?
Rochon: I’ll start, and then Dr. Reppas will certainly want to add in. When you’re starting to look at these problems, it’s important to think about what are some of the non-drug strategies that you might want to take. I think that’s what you’re just alluding to, Deborah.
For example, if a person is agitated, it’s really important to step back and start by thinking [about] what is it that’s causing this agitation. What is it in that person’s environment or the circumstances that [are] related to that agitation? And it’s usually very, very individual. I don’t think there’s one answer for what causes people to be agitated. It might be something related to a care routine, or it might be something related to noise, or the environment, or whatever it is.
Often, it’s in discussions, in some cases with the patient, the person involved, but often their caregivers or family members, to sort of understand what those issues are. Then, therefore, how might you address it? For example, maybe it’s about the environment, maybe it’s too loud, maybe it’s noisy, maybe they do better in a quieter, a calmer environment.
Some people respond well to things, like some people may really, really like music. How could you bring that in as something that might be helpful? Some people are very attached to animals or like pets—can that have a calming effect? Or maybe it’s about how people are approached; if it’s around caregiving what’s needed is, are there certain ways they like to be approached, do [they have] certain routines that work? It’s very much I think about understanding what the issues are, working with everyone to sort of understand how you might tailor approaches.
“I don’t think there’s one answer for
what causes people to be agitated.”
Being Patient: I’m glad that you pointed this out because my mom, who’s in a later stage of Alzheimer’s disease, has recently been looking for her parents. If you say to her, “Oh, no, your parents aren’t here,” she gets very agitated. But if you say, “Let’s finish this first, and then we’re going to find your parents,” she calms down immediately. I always think of this strategy. It’s like stepping into their world. Many people don’t feel great about it because you’re effectively lying, but it works.
Rochon: Sometimes that’s OK to do.
Being Patient: Sometimes, we just have to be more forgiving of ourselves and use the best strategy to make the person calm down and be less agitated. Because in the end, that’s better for them, right?
Reppas-Rindlisbacher: Yeah, and sometimes I think these things are not intuitive. There are specific programs that I like to refer caregivers to, like the Alzheimer’s Society, for example, where they can really learn, like, “How do I respond to certain, you know, requests or certain comments?” Where “I don’t know exactly how to respond,” and it seems to escalate things. So, I think the example that you gave was an excellent one. In terms of teaching caregivers better coping strategies and better communication strategies. That’s a really important step.
Being Patient: There are a lot of different reasons for agitation— sometimes it’s hallucination, right? That’s a tricky one because it’s not real. I mean, and maybe you could say my mom looking for parents is like a type of hallucination, but seeing things that aren’t there— that’s often something that we hear a lot about. Any recommendations for strategies there?
Reppas-Rindlisbacher: That’s definitely a tough one. At the beginning, I mentioned this group of symptoms called neuropsychiatric symptoms of dementia. That includes things like wandering or restlessness, agitation is one, and hallucinations are also one. That’s a really tough one because it can be really distressing.
Typically, what we do is we want to sort of approach that in a very patient-centered way and understand whether it’s distressing or not because some hallucinations actually aren’t distressing. They can be redirected in the way that you mentioned, about just sort of redirecting to something else. They’re not necessarily very distressing, but I think if they do become distressing, that’s the point in time where it’s important to talk to one physician about thinking about some of the medications.
Being Patient: In terms of benzodiazepines, can you tell us more about the side effects and what we should worry about in terms of medications?
Reppas-Rindlisbacher: The main reason why benzodiazepines are listed as potentially inappropriate under some of those criteria that Dr. Rochon mentioned is because they increase side effects that in patients with dementia can be potentially quite serious and life-altering. So, we know that there’s an association with falls and that’s probably related to being lethargic the next day. And a fall can, as I’m sure most of the audience knows, can be quite a devastating event. For an older person, it can lead to a hip fracture, for example, which can be life-altering.
Benzodiazepines are associated with increased confusion or associated with falls. This is less important for dementia, but there’s even been an association with new starts of benzodiazepines, increasing car accidents. The lethargy and the drowsiness that comes from these drugs does have significant side effects, but that has led for them to be on these lists of potentially inappropriate therapy.
Rochon: I think it impacts any older person. I mean, these are things that impact people in general as well.
“Benzodiazepines are associated with increased confusion or associated with falls”
Being Patient: What about their addictiveness? Is it like opioids, where it’s really hard to get off them? If medication is being administered for a longer period of time, is there a risk of withdrawal symptoms?
Reppas-Rindlisbacher: Yeah, absolutely. In that, there’s a tolerance that occurs. They’re not necessarily the same as opioids, but they do cause a tolerance in the brain that makes it very difficult, if one has been on these medications long term, to stop them suddenly. So, people can go through some withdrawal effects. increased anxiety, and insomnia.
Because of this, actually, when we are counseling patients to come off of these drugs, we would recommend doing it very, very slowly. I think, in fact, Dr. Rochon, I don’t know if you want to talk about the Empower brochures, but you know, we tend to follow like a very, very slow, like titrate titration approach where we decrease the drugs extremely slowly over long periods of time so that our patients don’t go through those withdrawal effects.
Rochon: I think this is something that’s really important to think about, that if you’re wanting to take people off of medications that they’ve been on for a period of time, like these in particular, it’s important that you do it in consultation with your clinician or care provider. That also speaks to something we could talk about around, you know if you want to optimize your medications for an older person, there’s some really nice guidance that’s out there that can help people think how to approach this. I think this is a big question for everyone right now.
People want to make sure they’re on the right medications for them, and where meds aren’t necessary, to think about the idea of de-prescribing. Some of the work that we’ve been involved with has created, I think, a really nice algorithm that people can follow called DRUGS, which, you know, kind of works well. It’s really important to discuss the goals of care as the starting point. What is it that’s important? What is it that matters? That’s something that really can vary from individual to individual.
The patient and the caregiver really need to have those discussions. Then you need to review the medications and look at what that person’s on because often they’re not just on a single medication. Often, there’s a series of medications: sometimes prescribed, sometimes over the counter. So, you really need to understand those, and then you need to think about these tools and frameworks.
We mentioned a couple. For example, the BEERS criteria, the guidance that clinicians can use. There’s another piece called STOPP/START. That is a similar kind of thing that’s used in Europe and more broadly. There are things that we’ve talked about related to things like prescribing cascades, but just to think if there are these meds that fit any of these kinds of lists of drugs, where there might be a potential concern, and then to think about the holistic approach. [Think] about how this relates to the whole family or the whole individual in their particular situation.
Then, in some cases, medications are deemed to no longer be required, and they need to be stopped. In some cases, it’s possible that some things need to be added. It’s very, very important, especially in the context we’re talking about, where people maybe have dementia, and they are on certain drugs, that those drugs are reviewed on a regular basis with the clinicians, just to make sure you know, the combinations are right.
“You need to review the medications and look at what that person’s on because often they’re not just on a single medication.”
Being Patient: For symptoms like agitation, what drugs are most often prescribed? Is there any protocol from the doctor’s perspective on how different medications are prescribed for treating these dementia symptoms?
Rochon: The first part is when somebody’s coming forward with symptoms, you want to think about potentially: what are some of the causes? What might be contributing to this? As we discussed earlier on, thinking about what some of the non-drug approaches might be, or in some cases, it’s also possible that some drugs that they’re on may be causing, for example, agitation. Sort of looking at those and adjusting in that regard. I mean, I think it’s really always important to start with the idea of thinking about the whole context, before you jump in to start adding something new.
Reppas-Rindlisbacher: I completely agree. I mean, I think first, of course, [we] need to ensure that a drug trial is necessary in the first place. The decision about which drug to prescribe is often driven by the kind of agitation or behavior that we’re talking about, right? Because agitation is a bit of an umbrella term, it can encompass so many different things. So, I would say that selecting an appropriate drug therapy for the patient’s specific symptoms is important.
If it’s really distressing hallucinations, then one drug might be more appropriate than another if it’s something like wandering. We know that drugs are less likely to be successful. It’s better to have environmental considerations about trying to reduce a behavior like wandering. I think it’s really important to think about the behavior that you’re trying to target because there’s not like a one-drug-fits-all approach, that’s for sure. That’s the case; I think, in general, we need to be patient-centered and think about the risks related to the behavior and whether the behavior is actually going to be helped by some of these drugs.
Being Patient: What are some of the strategies for asking your doctor about trying non-pharmacological interventions? You’ve mentioned materials you’ve developed, but give us a cheat sheet. I’m getting the feeling that you’re saying that we should go the non-medication way first, if possible, and then the medication route— is that right?
Rochon: That’s entirely right. When you’re going to your provider or doctor, I think you want to start with a conversation, “Here’s the challenges that we have. How can we potentially approach it and look and discuss the various different options?” It’s so important to have those conversations. It does have to start with, what are some of the non-drug approaches that you can use because you need to think about those [in perspective.] I mean, those can make a lot of difference.
Wherever possible, you need to figure out what some of the things are that are causing issues and how you can potentially manage those before you go into any conversation about drugs or even if you are going to be thinking about drugs. It’s just really important to have those conversations and have those dialogues and to be in close touch.
Being Patient: I’ve heard a lot from people in our community saying that being on certain drugs makes their loved ones quiet and sedated. While they’re not doing something that will harm themselves, they just exist. That’s kind of a moral judgment there, but is that good for someone if they’re kind of so medicated that they’re kind of just existing or just in a trance? Should we be concerned about that?
Reppas-Rindlisbacher: It’s a hard question, but it’s important that you bring that up, Deborah, because I think you alluded to this in your question about a lot of what we do, as geriatricians and treating patients with dementia, is informed by the values and preferences of that person and their caregivers. That’s a really important tenet of our specialty.
When we don’t have very good evidence, necessarily some trials, I think it’s up to us to give patients and families some of the risks and benefits but make our recommendations based on patient and family preferences. Depending on, you know, certain behaviors that might be more appropriate and depending on behaviors that might be less appropriate. In general, we always have to make sure the patient’s values and preferences inform our recommendations.
The other thing that’s important to mention is that things should always be reassessed, right? Anytime we’re starting a medication, it might have been the appropriate thing to start at one point in time, but if caregivers are noticing more side effects, or even if they’re not noticing more side effects, medications should always be reassessed at intervals because they may no longer be needed, as the dementia changes.
“In general, we always have to make sure the patient’s values and preferences inform our recommendations.”
Being Patient: How often should we be reassessing medications?
Rochon: Well, you could set some times as to when meds should be reevaluated. But also when things change, you know, if the person’s circumstance changed, a new medicine is being added. I think it’s really important to go back and to look at what’s already there. So, it’s important to do that on an ongoing basis.
Being Patient: I’m guilty of not really understanding what medications my mom is taking and for what. I mean, I think I have an inherent trust in her doctor, but I’m sure he’s not focused on whether she’s been on this drug for two or three years, right? I mean, that’s something that a care partner really needs to manage. If it’s working, then should we just stay on it?
Rochon: If you know it’s working, that’s good, but I still think it’s important to go back and reevaluate. Because sometimes, maybe it’s working, but maybe there’s an opportunity to adjust a dose or something that you might want to do going forward— because circumstances can change. I do think it’s important to have these sorts of ongoing discussions.
“If you know it’s working, that’s good, but I still think it’s important to go back and reevaluate.”
Being Patient: Tell us about some of the resources you’ve mentioned so that we can direct people to find and use them. What were the criteria for medicines not recommended for older adults?
Rochon: The things we’re talking about are the different sorts of frameworks and guidance that are out there around medications, and those are publicly available. You can find those and a variety of different sites. We’re talking about one of the most widely known ones called the BEERS criteria and another is the STOPP-START criteria.
Then another one that we find is really useful that we’ve developed. Dr. Reppas, myself, as well as some colleagues, is one that’s called a DRUGS approach that we’ve talked about in some of the work that we’ve done, which I think is helpful for family members to look at when they’re thinking about you know, meeting with the physician and having discussions about whether the right combination of medications for the individual that they’re caring for.
Being Patient: Before you go, give us a cheat sheet for going to the doctor’s office and talking about symptoms. What should we be asking our doctor to treat agitation symptoms? What are the first few questions we should be asking?
Rochon: If you’re coming in with a cheat sheet, I think you should also be coming in with a bag with all the medications that somebody’s currently on. Because I think that is often something that, even doctors are supposed to have that information, [but] they don’t always have it, especially over-the-counter type medicines.
I find it’s also really important for families and caregivers to have a note of when the medication was started, why it was started, and who started it because that information can get lost. That can relate, you know, further down the line to understanding side effects that you might not have anticipated. I like people to come in with some of that basic information when walking into the office.
Reppas-Rindlisbacher: I think that’s an excellent start. I would just add other questions like: are the symptoms that I’ve described? Are they likely to respond to these drugs? Because, like I said, some symptoms are more and less likely to respond. So, I think that’s an important question, obviously asking about the side effects, asking about what side effects to look out for, and also what benefits to look out for so that the next time you meet with your healthcare provider, physician, nurse practitioner, you know, what you’ve been asked to look for, and then you can inform good decision making about whether or not the drug is working or whether the dose needs to be adjusted. I think that’s also really important.
Reporting by Simon Spichak. Live Talk produced by Katy Koop.


I would love to introduce you to Audivi Memory Banks, an app I started based on my experience taking care of my mom with dementia. Playing her memory bank was such a great way to redirect & reduce the challenging symptoms (and give me, the caregiver, a break).
Kristin, using tools like apps and music to spark memories shows real promise for redirecting challenging dementia behaviors. This article shares more on that approach: https://www.beingpatient.com/reminiscence-therapy-my-house-memories-app-dementia/. Thank you for sharing your app. Wishing you the best with that meaningful work!
Benzodiazepines are only appropriate for pre-surgical prep. They are not only inappropriate for anyone over 65, but for anyone any age. They kill patients due to falls, homicide, accidents, & suicide & cause dementia & any doctor who prescribes them routinely is crazy & is playing roulette with his license. Check this out at the benzodiazepine information coalition on the web.