Most FDA-approved Alzheimer's drugs are designed just to address symptoms. Now, a new wave of treatments targeting the disease's hallmarks is in development. Here's how they're different.
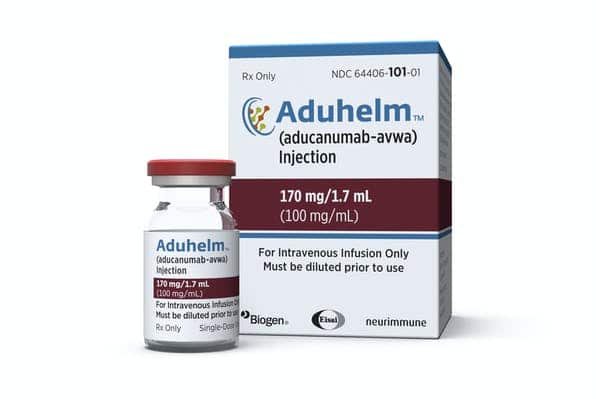
What’s the difference between treating Alzheimer’s symptoms and modifying the disease? Despite decades of research, the underlying cause of Alzheimer’s continues to evade scientists. Until recently, the only drugs available to patients targeted the symptoms of the disease, rather than underlying pathology. That’s why the FDA approval of the anti-amyloid drug Aduhelm this summer was such a significant milestone: Hailed as the first drug with the potential to modify the course of the disease’s pathology, Aduhelm (aducanumab) is designed to slow disease progression. The drug’s efficacy has been the source of great controversy, but other anti-amyloid drugs designed to function similarly — addressing the disease itself, not just the symptoms — are close behind it in the drug development pipeline. (In February 2024, Biogen took Aduhelm off the market indefinitely.) Two more, lecanemab and donanemab, recently received breakthrough status, meaning they’ll be fast-tracked for review by the FDA.
But what is the clinical relevance of the distinction between treating symptoms and modifying disease? And is this paradigm even useful?
Treating Alzheimer’s symptoms
The symptoms of Alzheimer’s often appear 10 or more years after the disease itself starts. By then, progressive cell death causes cognitive impairment, confusion, memory problems, trouble sleeping, and changes in mood or personality. Catching these symptoms at an earlier stage, at the first signs of mild cognitive impairment, is crucial for implementing lifestyle interventions, prolonging the quality of life, and preserving cognitive function for longer.
Several drugs are approved to treat these cognitive symptoms. For people with mild, and in some cases moderate, Alzheimer’s (depending on each drug’s specified uses), these symptomatic treatments can have a major impact on day-to-day quality of life.
However, the disease will continue to progress, and at moderate and severe stages, these treatments become less effective as brain cells continue to die.
While symptomatic treatments aren’t intended to target Alzheimer’s root causes, some have shown the ability to go beyond their initial “band-aid” intentions, and actually potentially slow the disease’s progression.
Galantamine (brand name Razadyne) is an Alzheimer’s drug developed with the intent to treat cognitive symptoms, and approved for by the FDA this purpose 18 years ago. A recent study published in the journal Neurology found that, compared to other symptomatic treatments, Galantamine may also reduce the risk of severe dementia.
While researchers have yet to determine precisely why this is the case, there is some evidence that this drug increases amyloid plaque removal in the brain, just like the new wave of disease-modifying anti-amyloids that are currently in development. Whether or not this approach is ultimately the right one when it comes to stopping Alzheimer’s in its tracks is still an unknown.
Once researchers learn more about this mysterious disease’s underlying causes — either validating or moving on from the “amyloid hypothesis” under which drugs like Aduhelm, lecanemab and donanemab are being developed — there will be other hurdles to overcome. For one, the only available one of these so far, Aduhelm, is so prohibitively expensive that the cost of Medicare premiums for many Americans have gone up just to accommodate it.
Many Alzheimer’s experts suspect that there is no “magic bullet” to Alzheimer’s due in part to its complex nature. There is a lot of hope for new disease-modifying treatments, but treating and managing Alzheimer’s may require a personalized combination of treatments — those that modify the disease itself as well as drugs that treat its symptoms.
UPDATE: 3 March 2024, 9:28 P.M. ET. In February 2024, Biogen took Aduhelm off the market, citing financial concerns. Although the drug did receive accelerated, conditional FDA approval for the treatment of early Alzheimer’s disease in 2021, it is no longer available to new patients. The company announced it would sunset trials in May 2024 and cease supplying the drug to current patients in November 2024.