The symptoms that characterize Alzheimer’s disease — like memory loss, impaired thinking, even personality changes — aren't just a normal part of aging. What exactly is Alzheimer's, and how do doctors diagnose it?
Dementia is a term used to describe a set of symptoms: memory loss and other cognitive issues. The most common disease that causes these symptoms is called Alzheimer’s. It accounts for 60 to 80 percent of dementia cases and usually occurs in people 65 and older. But what is Alzheimer’s disease, exactly? This neurodegenerative dementia is characterized by abnormal protein clumps and tangles in the brain. It causes problems with memory, thinking and behavior.
And do doctors know when someone has Alzheimer’s? Diagnosing it can be tricky, as there are a lot of other types of dementia that look similar. Diagnosing Alzheimer’s disease will require a battery of tests to confirm the presence of those problematic proteins in the brain and to rule out other, similar diseases.
Despite common misconceptions, those symptoms that characterize Alzheimer’s — memory loss, impaired thinking, personality and mood changes — aren’t just a normal part of aging. Something’s going wrong inside the brain. Here’s a breakdown of the basics.
Early signs of Alzheimer’s disease
There are many different early signs that someone might be developing Alzheimer’s — though some of these symptoms could also be signs of other health problems. Often, the person experiencing these problems might be unaware, and patients’ families or loved ones are the first to notice.
- Memory lapses. Often, people in the early stages of the disease will develop some problems with memory, forgetting names, dates, or words for everyday objects.
- Difficulty paying attention. Some people might develop problems focusing on familiar tasks, leading to more difficulty completing tasks at work or home than usual.
- Problems with navigation. The part of the brain that starts to die first in Alzheimer’s is called the hippocampus, which is essential for navigation. Tony Gonzales, a third-generation Mexican American, got lost driving home from work. For him, that was the first sign that something was off.
- Trouble with math and finances. Family members might find that their parents have suddenly become bad at managing their finances or are victims of a financial scam.
Changes in personality or behavior. People with Alzheimer’s may develop anxiety or other personality changes, like becoming more irritable or having more mood swings.
Alzheimer’s disease symptoms and stages
Because Alzheimer’s disease is a progressive degenerative disease, symptoms begin mildly and get worse over time. There are seven stages of Alzheimer’s disease, each with their own set of symptoms. (You can download the 7 stages chart and how to manage each stage here.)
As Alzheimer’s disease advances, so do the symptoms. Common Alzheimer’s symptoms include: forgetting names and words, losing things, difficulty planning and organizing, poor short-term memory, difficulty with math, forgetting details of your life, disorientation, mood and behavior changes including depression, withdrawal and agitation, inability to recognize faces, false suspicions about people, and eventually difficulty performing everyday tasks like dressing, walking, speaking and swallowing.
People with Alzheimer’s disease don’t always recognize that they are having memory issues. That’s why it’s important for loved ones to point out their concerns and act as a healthcare advocate at their doctor’s appointments.
How Alzheimer’s changes the brain
Changes in the brain begin to occur decades before the symptoms of Alzheimer’s disease develop.
A recent study published in the New England Journal of Medicine measured the levels of key brain biomarkers — beta-amyloid plaques and tau protein tangles — in the cerebrospinal fluid of 648 cognitively normal participants over twenty years. In the patients that developed Alzheimer’s, the scientists noticed changes in amyloid 18 years before diagnosis, changes in tau 11 years before diagnosis, and signs of neurodegeneration and brain injury nine years before diagnosis.

The Alzheimer’s Association has developed diagnostic criteria that rely on these biomarkers, although an accurate diagnosis still requires a full workup from a clinician after symptoms first appear. Beta-amyloid and tau aren’t perfect predictors of Alzheimer’s disease — they are also present in many healthy, older individuals and other forms of dementia.
However, scientists still don’t fully understand why these changes in the brain occur before the symptoms of Alzheimer’s disease. Some researchers believe that amyloid and tau are key causes, while others suggest that viruses or problems with the immune system might be the real culprits.
Why Does Beta-Amyloid Build Up in the Brain—And Is It Reversible?
How is Alzheimer’s disease diagnosed?
The first step to diagnosing Alzheimer’s involves ruling out other less-serious conditions.
Dr. Sharon Cohen, clinician and director of the Toronto Memory Program, told Being Patient that this involves checking for low thyroid or vitamin B12 levels in the blood. This could cause temporary impairment and may be caused by another condition. A CAT scan or MRI can help rule out strokes or tumors.
Clinicians will also speak to a “knowledgeable informant” — a family member, spouse, or caregiver — to get an accurate history.
After that, clinicians may run standardized cognitive tests. Even expert clinicians cannot rely on the results of these cognitive tests alone. “When we diagnose Alzheimer’s disease without a confirmatory test, we are wrong about 30 percent of the time,” Cohen said. Several blood tests on the market can help doctors screen for or rule out the disease by looking for blood biomarkers of Alzheimer’s.
At this stage, if Alzheimer’s is still a possibility, a clinician can order one of three tests to make a more certain diagnosis. These tests are not diagnostic tests, but they provide doctors with information about whether a patient has beta-amyloid plaques and tau protein tangles in the brain.
Taken together with the other battery of cognitive tests, these tools can help a doctor make a more accurate diagnosis. Some patients might need multiple types of biomarker tests before their doctor is certain they have Alzheimer’s.
Cerebrospinal fluid test
This method involves using a lumbar puncture to extract a small amount of cerebrospinal fluid to test the levels of beta-amyloid or tau proteins to see if they are indicative of Alzheimer’s pathology. The cost of the lumbar puncture is covered by Medicare.
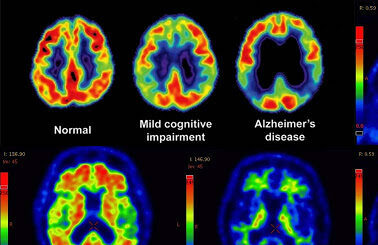
Amyloid PET Scan
An amyloid PET scan is another way to look for beta-amyloid plaques in the brain.
This test involves injecting a special tracer molecule into the bloodstream that binds to beta-amyloid in the brain and blood vessels. When the patient goes through a PET scan, this tracer allows a radiologist to determine whether someone has high levels of beta-amyloid plaques indicative of Alzheimer’s disease. Amyloid PET scans are now covered by Medicare.
Blood tests
Blood tests that measure the levels of various biomarkers in the blood can also be used as a porxy for measuring Alzheimer’s and tau pathology in the brain. These tests are currently not covered by Medicare and may cost up to $300 to $1500 out-of-pocket.




Learning what I can to help my husband and myself, so I know what to do to make this easier for him and for his family.
I never thought that we’d be going down this road. My husband is meeting many of the problems listed.
Hi LaNell, thank you for being here! Happy to be able to connect you with science-backed journalism on these topics.